Ethnicity
There have been decades of research highlighting ethnic inequalities in the prevalence of mental health conditions and across all aspects of the mental health system, though the quality of evidence varies across different ethnic groups and services (Kapadia et al., 2022).
Ethnicity is a complex and subjective method of identifying population groups (Raleigh & Holmes, 2021). Within each of these groups, there are variations in culture, country of origin and experience. Ethnic inequalities in health can accumulate over the life course and are ‘exacerbated in older ages’ (Stopforth et al., 2022).
Much of the data collected on mental health inequalities uses aggregated ethnic group categories, which is likely to mask differences in the experiences and outcomes of people falling within broad ethnic groups. Past needs assessments have highlighted that the lack of systematically collected data on the mental health of people from ethnic minority backgrounds (Hartley et al., 2019).
The 2014 adult psychiatric morbidity survey showed that the proportion of adults experiencing common mental health conditions in the past week varied by ethnic group for both women and men (NHS Digital, 2020), with rates of common mental health conditions being amongst Black women than all other groups.
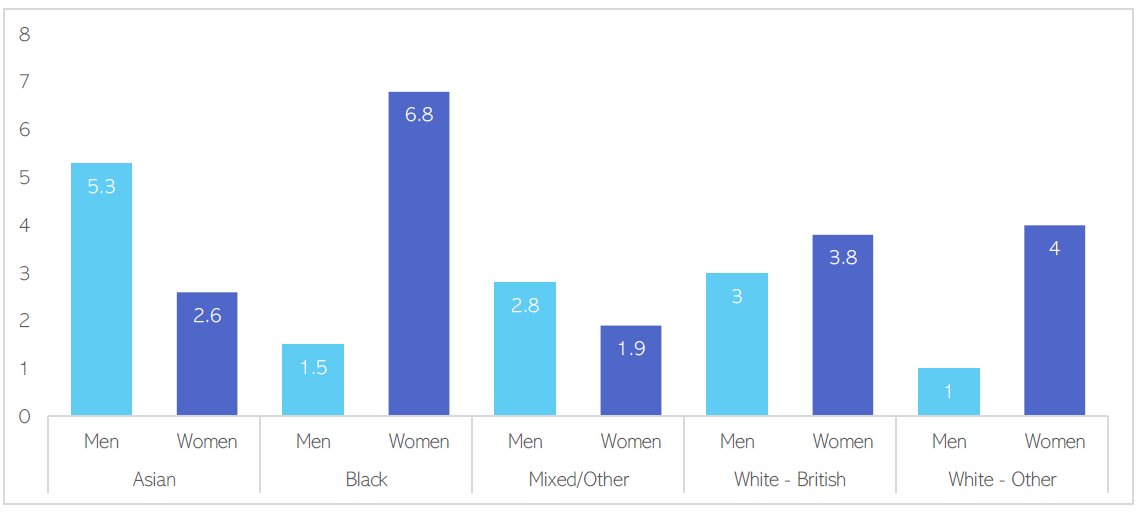
Figure 15: Percentage rates of common mental health conditions by ethnic group and sex. Data source: (NHS Digital, 2020)
Relative to White British people, people from other ethnic groups are more likely to be diagnosed with severe mental illnesses (SMI), including schizophrenia and affective psychoses (Halvorsrud et al., 2019). Similarly, migrants are more likely to be diagnosed with psychoses than those people who are not immigrants (Halvorsrud et al., 2019).
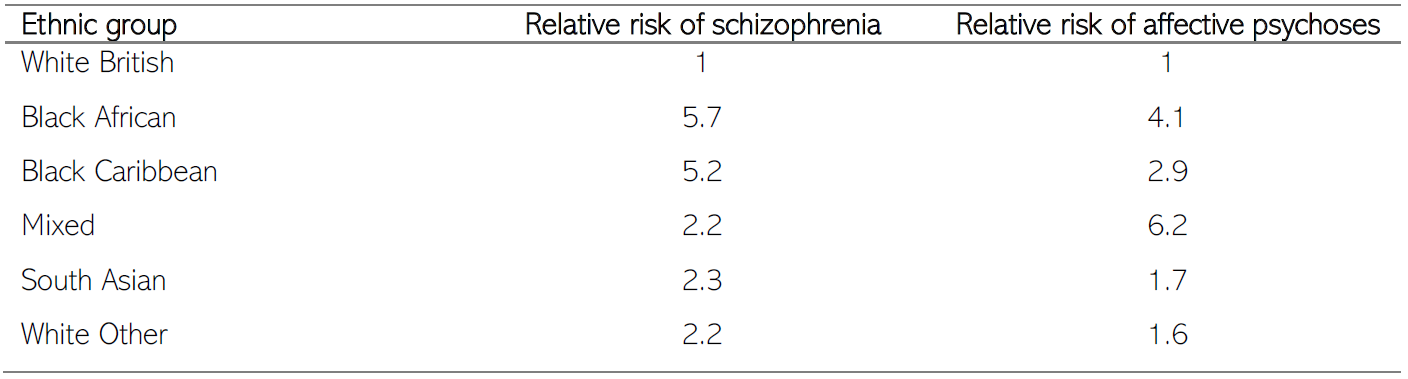

Table 5: Relative risk of diagnosis of schizophrenia and affective psychoses of ethnic groups. Data source: (Halvorsrud et al., 2019)
- People from ethnic minority groups may have better mental health when living in areas with higher proportions of people with the same ethnicity as them (known as higher ethnic density) (Bécares et al., 2018). Ethnic density is protective against psychosis and suicidal ideation; and may be protective against anxiety and depression.
- Ethnic density is protective against psychosis; and may be protective against suicide and self-harm, though data on this is limited as studies having only been carried out in South London.
- Evidence on the impact of ethnic density on the prevalence of anxiety and depression is mixed, with studies suggesting it may have a neutral or protective effect.
Local population
In Cambridgeshire and Peterborough, the proportion of the population who identify as ‘Asian, Asian British, or Asian Welsh’ is substantially higher than the national and East of England averages.
- The proportion of the ‘White’ ethnic group in East Cambridgeshire, Fenland, and Huntingdonshire is substantially higher than the national average, whereas the proportions of ‘Asian, Asian British, or Asian Welsh’ and ‘Black, Black British, Black Welsh, Caribbean, or African’ ethnic groups are lower than the national averages in these areas.
- In South Cambridgeshire, the proportions of all ethnic groups are similar to East of England.
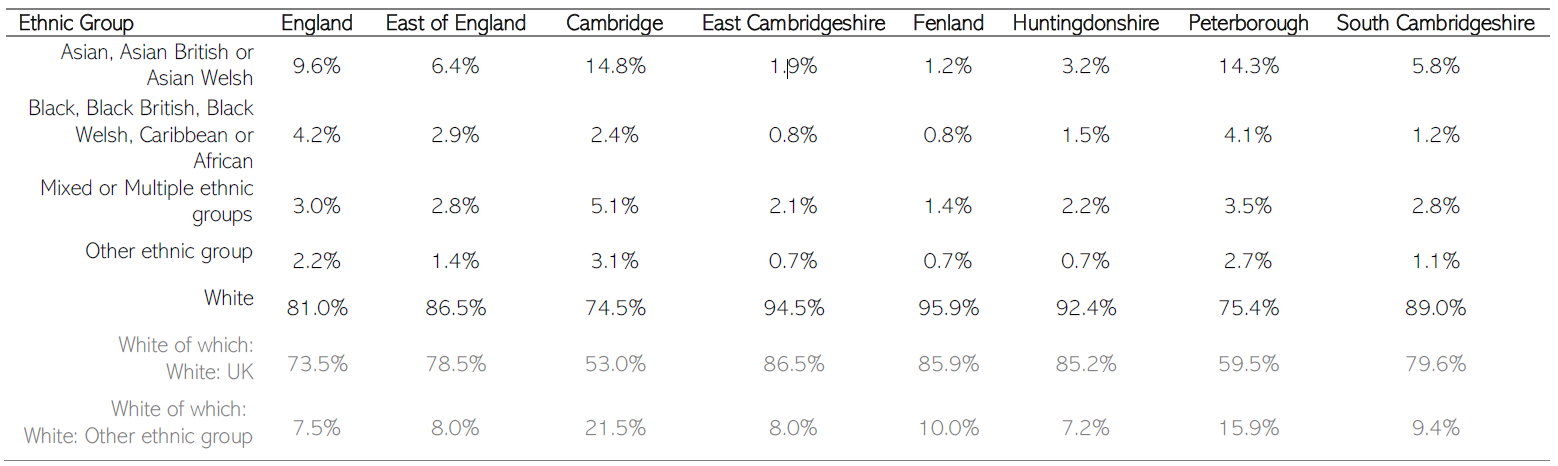
Table 3: Percent of population by ethnic group, Census 2021. Data source: Cambridgeshire Insight
During the 2021/22 academic year, 38% of school pupils in Cambridgeshire and Peterborough classify themselves as belonging to an ethnic groups other than White British (Department for Education, 2023a). The proportion of school pupils from Asian (17.5%) and Black (4.8%) ethnic groups was substantially higher in Peterborough than in Cambridgeshire (5.4% and 1.5% respectively).
Gypsy, Roma and Traveller communities
Note on terminology
- The term Gypsy, Roma and Traveller is used describe a range of ethnic groups or people with nomadic ways of life who are not from a specific ethnicity. It is useful to differentiate the specific experiences of the following groups (Women and Equalities Committee, 2019):
- Gypsies, which includes English Gypsies, Scottish Gypsy/Travellers, Welsh Gypsies and other Romany people.
- Irish Travellers, who have specific Irish roots.
- Roma, who are more recent migrants from Central and Eastern Europe.
- Within each of these groups, there are variations in culture, country of origin and experience.
- Whilst some people find the term ‘Gypsy’ offensive, many others feel proud to use this word, hence it has been included when appropriate in this report (Women and Equalities Committee, 2019).
- 3,214 people in Cambridgeshire, and 1,565 in Peterborough, identified as being Gypsy, Roma or Traveller in the most recent census. However, census figures are widely recognised as an undercount (Friends Families and Travellers, 2022).
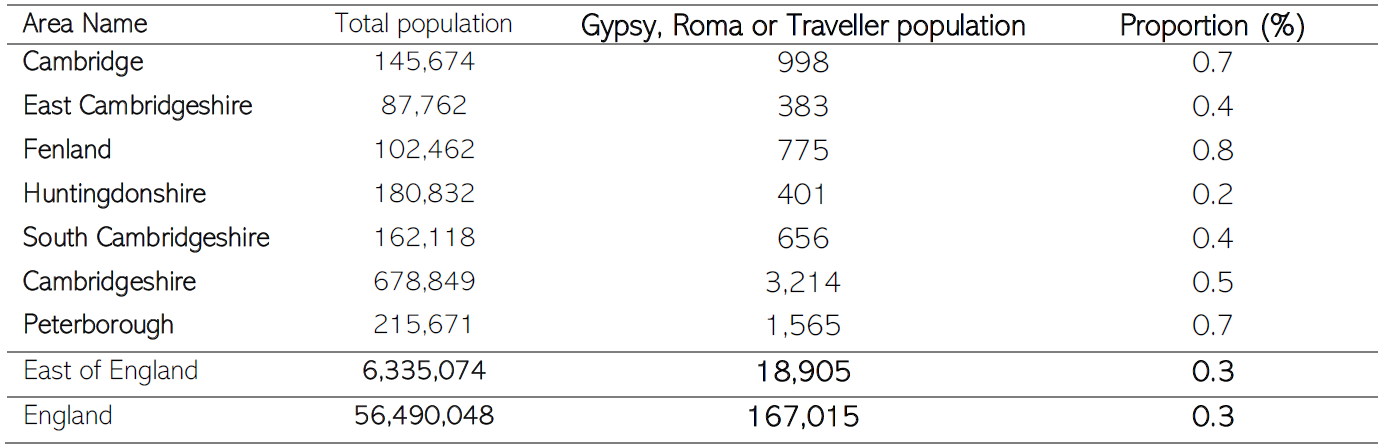
Table 4: Number and proportion of the population from Gypsy, Roma or Traveller groups. Data source: NOMIS
- Around a quarter of Romany Gypsy and a quarter of Irish Travellers groups in the UK live on Traveller sites in caravans or chalets (Friends Families and Travellers, 2022). Across Cambridgeshire and Peterborough, there are increasing numbers of people living in Traveller caravans (DLUHC, 2022b). Note that this data source is recognised as an undercount of true figures (Friends Families and Travellers, 2022).
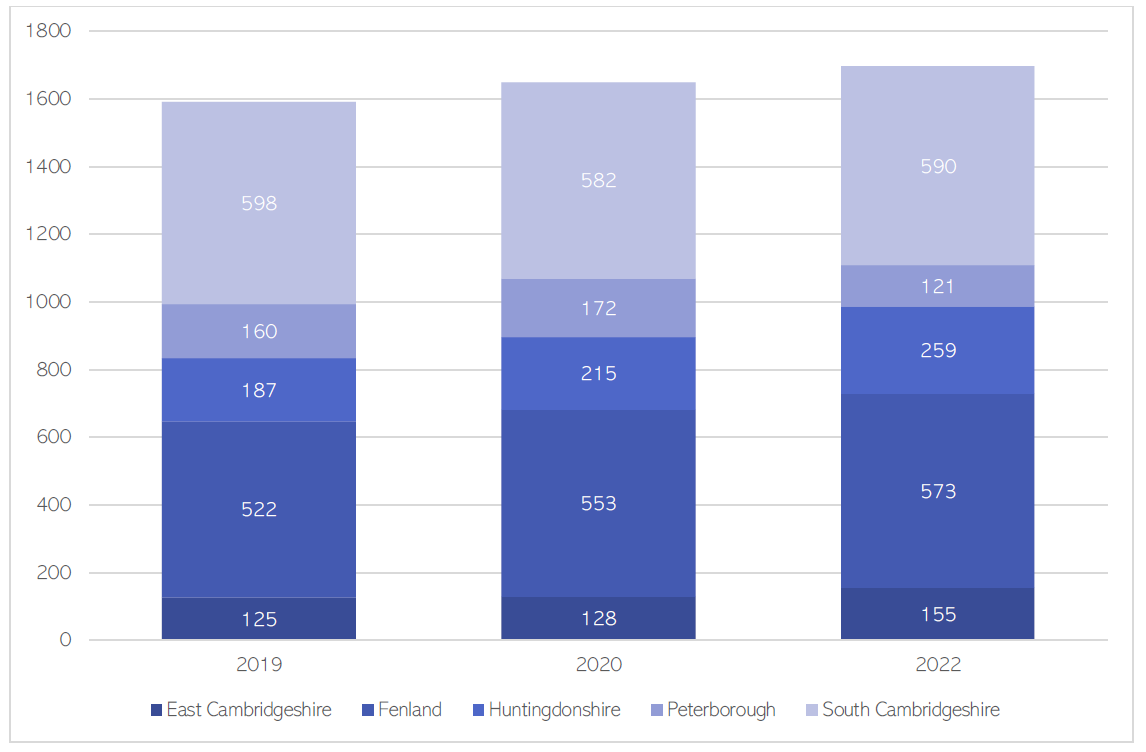
Figure 14: Total number of Traveller caravans across C & P recorded in January each year from 2019 to 2022. There are no caravans recorded in Cambridge. Data source: (DLUHC, 2022b)
Risk factors for poor mental health
Health inequalities associated with ethnicity result from a complex interplay of social and economic inequalities, shaped by racism and discrimination (Nazroo, 2022). Whilst they are closely related to socioeconomic inequalities, they are not fully explained by socioeconomic factors (Nazroo, 2022).

Figure 16: Dimensions of racism and how they can lead to inequalities in mental health. Adapted from: (57)
- Racial harassment, experiences of discrimination, and fear of experiencing racial harassment have cumulative impacts on physical and mental health [(Nazroo, 2022),(Stopforth et al., 2022)]. They can lead to ‘more traumatised and less confident, informed, resourceful and resilient communities’ (Bhui et al., 2018). The Centre for Mental Health states that tackling racism is one of their top priorities for reducing inequalities in mental health (Centre for Mental Health, 2022b).
- People from ethnic minority backgrounds are more likely to experience many environmental risk factors for poor mental health (see Chapter 1 as to why these factors are important). The relationship between these wider factors and health inequalities is unlikely to apply equally across all ethnic groups (Raleigh & Holmes, 2021).
- One environmental factor linked to both health and ethnic inequalities is deprivation: larger proportions of people from most ethnic minority groups compared to White British groups live in the 10% most deprived areas of England, including 31.1% of people from Pakistani backgrounds and 19.3% of people from Bangladeshi backgrounds, (Raleigh & Holmes, 2021).
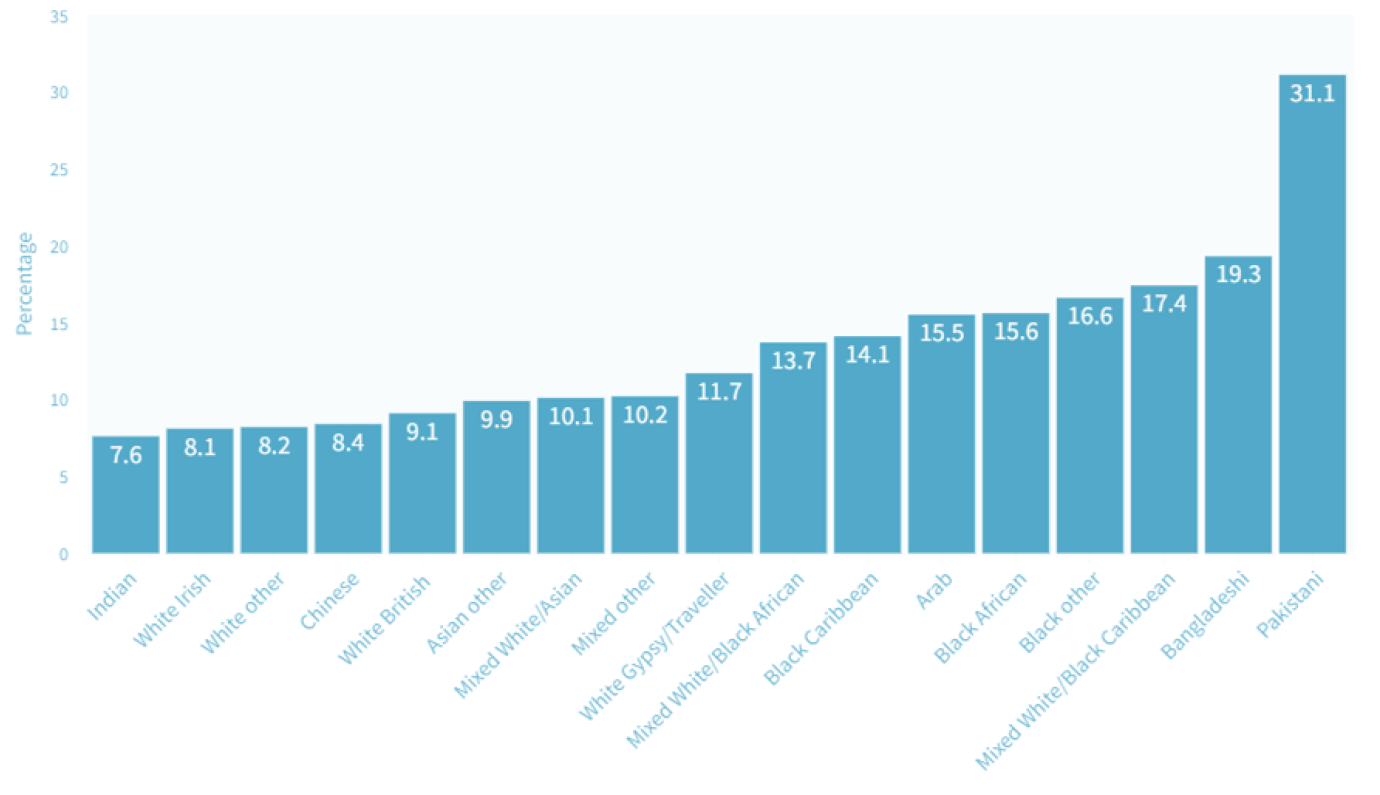
Figure 17: Proportion of ethnic group populations living in the 10% of most deprived neighbourhoods in England, 2019. Image source: King’s Fund
There are marked ethnic inequalities in physical health, which is closely linked to mental health (Nazroo, 2022). People from Gypsy, Irish Traveller, Bangladeshi and Pakistani backgrounds have the poorest physical health outcomes across a range of measures (Raleigh & Holmes, 2021). The graph below shows that 20% of Bangladeshi people in their 50s rate their health as being ‘fair’ or ‘poor’, a comparable proportion to White British people in their 80s.
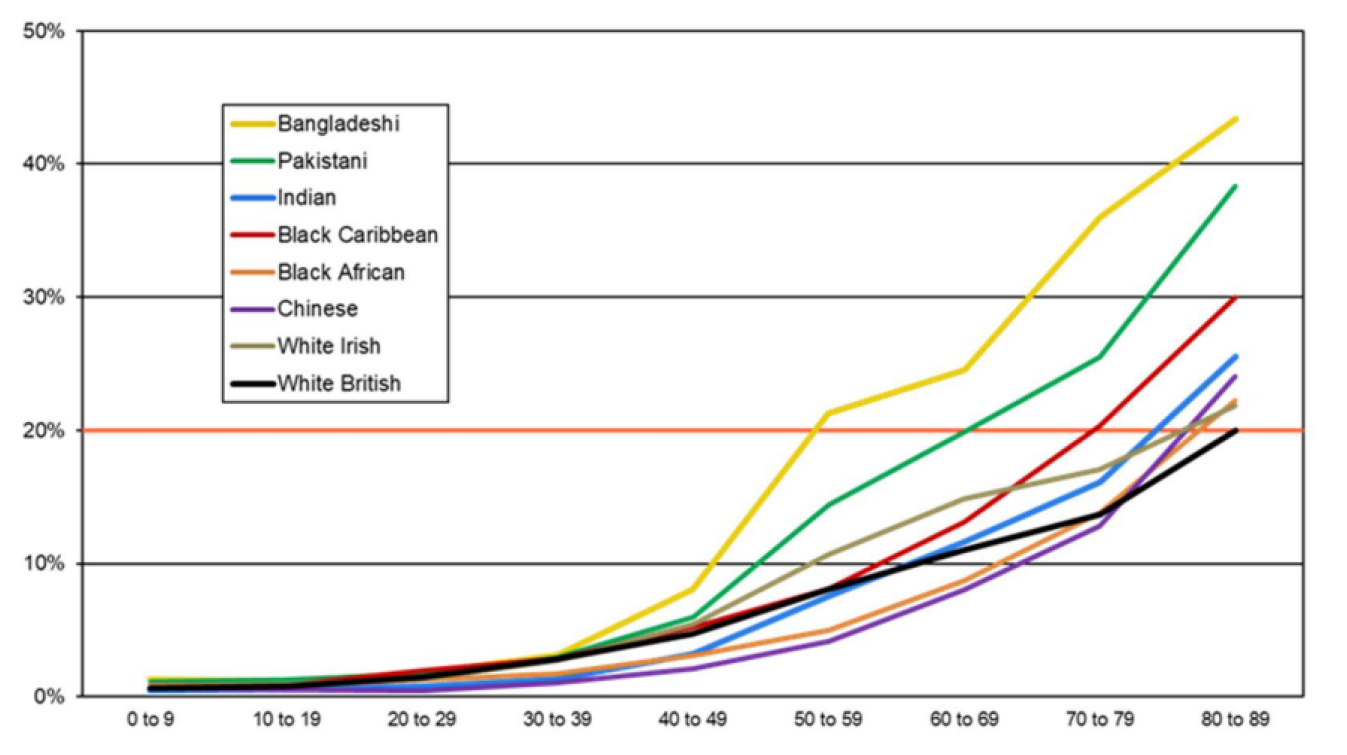
Figure 18: Ethnic differences in the proportion of people rating their health as ‘fair’ or ‘poor’ in the 2011 census. Source: (Nazroo, 2022)
Access
Nationally, people from Asian/Asian British, White Other and Black/Black British ethnic groups are less likely to receive mental health treatment for common mental health conditions than people from White British groups (Ahmad et al., 2022). Rates of mental health treatment are lowest amongst Black/Black British people.
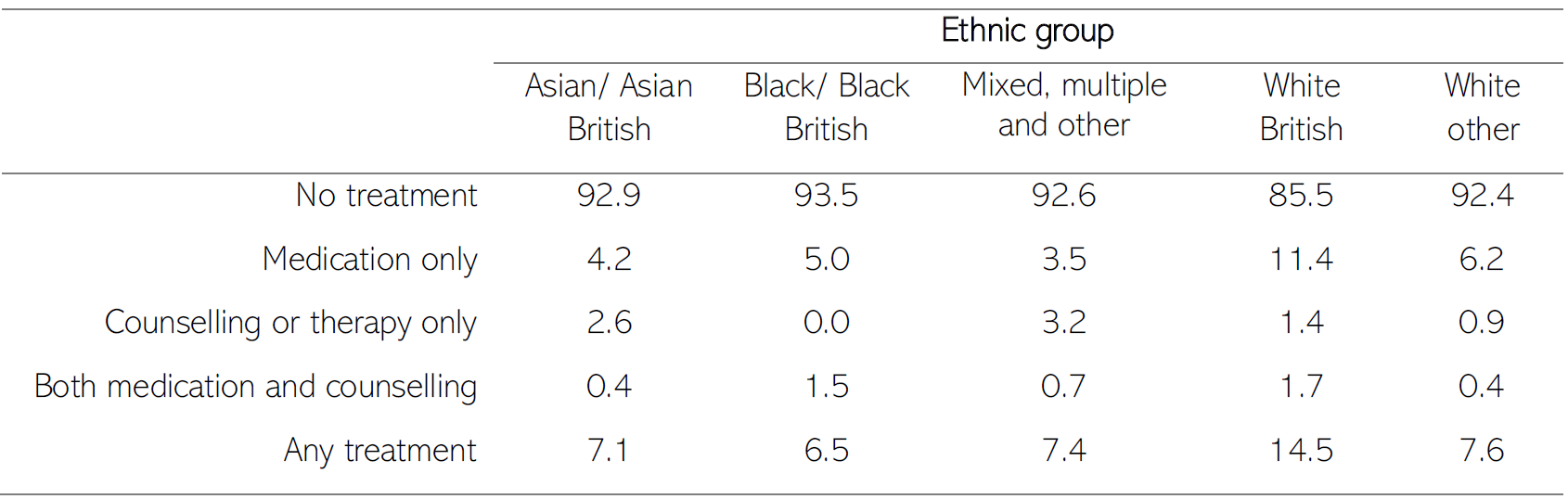
Table 6: Proportion of people who have received treatment for a mental health or emotional problem, by ethnic group. Data source: (NHS Digital, 2014)
People from ethnic minority groups are consistently less likely to access and receive appropriate mental health support from primary care (Ahmad et al., 2022). Barriers to accessing mental health services faced by people from ethnic minority groups include:
Healthcare system barriers to accessing mental health support
- People from ethnic minority backgrounds are less likely to be diagnosed with common mental health conditions (Bogdanova et al., 2022) and are less likely to be referred to specialist mental health services at earlier stages of distress. For example, although the prevalence of obsessive compulsive disorder (OCD) is similar across ethnic groups, adults and teenagers from ethnic minority groups are underrepresented in specialist OCD services (Fernandez de la Cruz et al., 2015).
- Language barriers and lack of access to interpreter services can prevent people from accessing mental health support [(Kapadia et al., 2022),(Memon et al., 2016)].
- Evidence of whether some ethnic groups are more likely to access Talking Therapies services is inconclusive (Kapadia et al., 2022). However, self-referrals and GP referrals into Talking Therapies are lower among migrants who have lived in the UK for less than 10 years (Bhavsar et al., 2021).
- Some people may experience language barriers.
- Research suggests that older people from ethnic minority backgrounds may face specific barriers in accessing health services due to digital exclusion and digital applications not being available in different languages (Kapadia et al., 2022).
Individual barriers to accessing mental health support
- Studies with people from a range of ethnic backgrounds (including Indian, Pakistani, Bangladeshi, Black British, Black African) have reported that a lack of trust in healthcare professionals is a key reason as to why people do not seek help from mental health services, including people feeling that professionals do not understand racism (Kapadia et al., 2022).
- Cultural background and identity can define ‘acceptable’ ways of managing mental health difficulties (Memon et al., 2016). For some communities, stigma around mental health can impact the whole family of someone with a mental health condition (Memon et al., 2016).
Pathways to accessing care
- People from some ethnic groups are more likely to enter the mental health system through after being detained under the Mental Health Act, rather than via less coercive pathways.
- National research shows that these inequalities have persisted for at least the past 60 years and are present even after adjusting for deprivation (Weich et al., 2017).
- The greater risk of compulsory treatment may reflect ‘wider issues of disempowerment, lack of trust, social exclusion and a lack of political influence, evident most in ethnic minority groups but common in other patient groups who complain of exclusion and dissatisfaction with care. These complaints are heard in local patient groups and are rarely captured in the research or professionalised evidence’ (Bhui et al., 2018).
- Relative rates of detention under the Mental Health Act in Cambridgeshire and Peterborough are, compared to people from White ethnic groups (NHS Digital, 2022):
- 3 times higher for people from Black ethnic backgrounds.
- 5 times higher for people with a mixed ethnic background.
- 2 times higher for people from ‘Other’ ethnic backgrounds
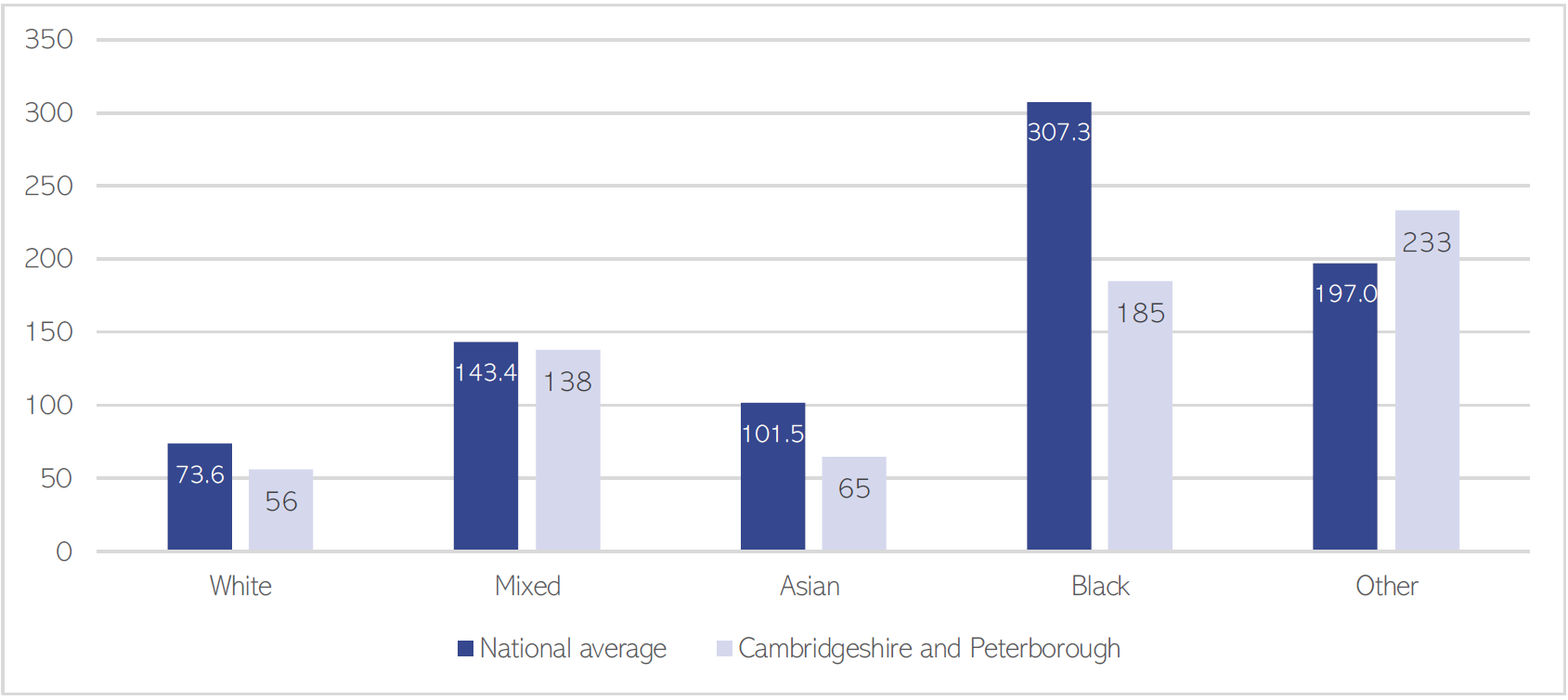
Figure 20: Rates of detention under the Mental Health Act 1983 per 100,000 of the population in 2021/22, by ethnic group. Data source: (NHS Digital, 2022)
- National data shows that migrants are 1.5 times more likely to experience compulsory inpatient admission to mental health units than people who are not migrants (Barnett et al., 2019).
- Compared to White ethnic groups, rates of compulsory inpatient readmission to mental health services are (Barnett et al., 2019):
- 3 times higher in people from any Black background.
- 3 times higher in people from Black Caribbean backgrounds.
- 3 times higher in people from South Asian backgrounds.
- Young people from Black, Asian and Mixed ethnic backgrounds are around twice as likely to be referred to mental health services through social care or youth justice services relative to primary care, compared to White British young people [(Edbrooke-Childs & Patalay, 2019), (Chui et al., 2021)]
- Compared to White British children, Black children are 10 times more likely to be referred to children and young people’s mental health services through social services rather than via their GP (Mckeown, 2023).
Experience
- Poor relationships between people from ethnic minority groups and mental health services can lead to a spiral of mistrust affecting experience and treatment outcomes (O’Brien et al., 2009).
- Black people, and people from Mixed Black and White ethnic backgrounds, report higher levels of unfair treatment by mental health services and staff than White patients (Henderson et al., 2015).
- Young people from minority ethnic groups often feel that their mental health needs are taken less seriously than those of their White peers (The Student Commission, 2022).
- White healthcare professionals can be perceived as being ‘unable to understand or sympathise with the realities and experiences’ of people from an ethnic minority background (Memon et al., 2016).
- Clinicians have greater uncertainty in diagnosing depression and emotional problems in Black patients and patients from other ethnic minority groups, compared to when diagnosing White patients (Bignall et al., 2019).
- People from Black, Bangladeshi and Pakistani backgrounds experience less continuity of care in primary care than White patients (Gopfert et al., 2021). Most young people (aged 16 to 24) from minority backgrounds have below average experiences of primary care services (Mckeown, 2023).
- Many staff in the NHS experience racism (Ramamurthy et al., 2022). In the East of England in 2021:
- White applicants for NHS roles were 2.0 times more likely to be appointed from shortlisting than ethnic minority applicants (NHS England, 2023b).
- 18% of ethnic minority NHS staff reported having experienced abuse or harassment from other staff in the past 12 months, compared to 8% of White staff members (NHS England, 2023b).
Outcomes
‘Traumatic, inappropriate and discriminatory experiences of services can have a detrimental impact on chances for recovery, particularly if the same risk factors of bereavement, family breakdown, incarceration, poverty and exposure to racism continue to be present’ (Bignall et al., 2019).
Outcomes from Talking Therapies (previously known as IAPT) vary by ethnic group (NHS Digital, 2021):
- Local data highlights that people from Asian or Asian British backgrounds have poorer rates of recovery and improvement after finishing treatment through these services, and have higher rates of deterioration, when compared to the national average.
- People from ‘Unknown’ and ‘Other’ ethnic groups also have poorer outcomes.
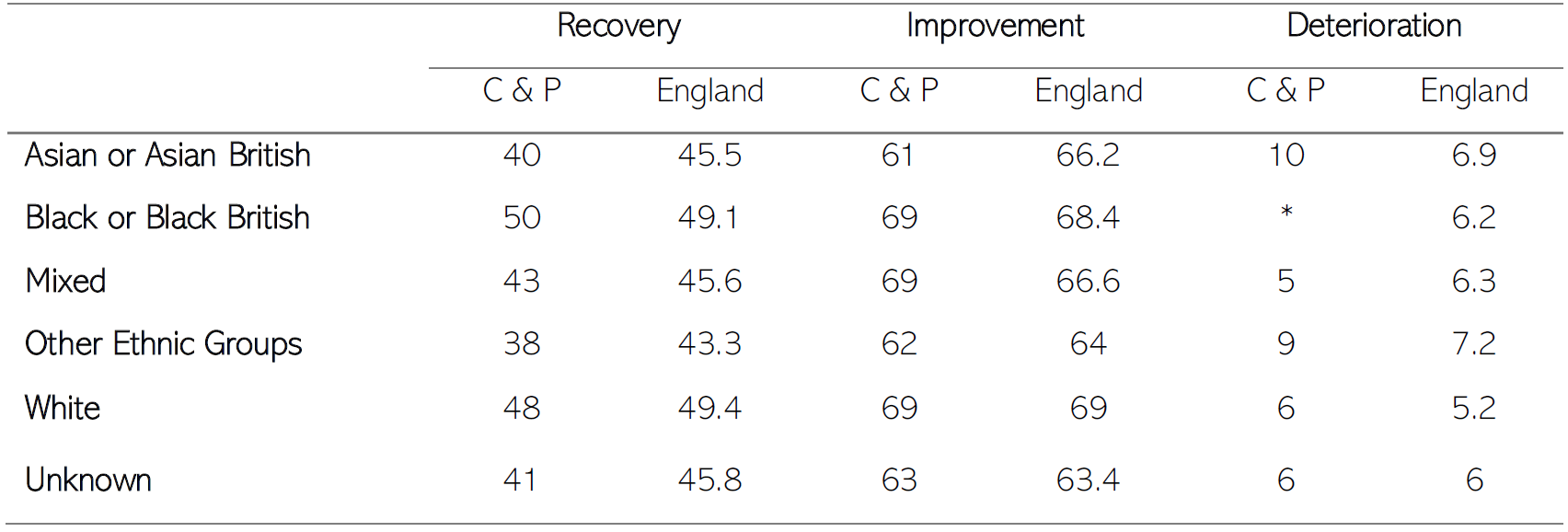
Table 8: The proportion of people who have consistent recovery, improvement and deterioration in their mental health for referrals for IAPT who finished treatment in 2020/21, across C & P and England. Data source: (NHS Digital, 2021)
The * indicates a count based on less than 5 individuals, which has been suppressed to protect patient confidentiality. Full definitions of ‘recovery’, ‘improvement’ and ‘deterioration’ are provided by NHS Digital.
- Compared to people from White ethnic groups, people from ethnic minority backgrounds are more likely to report having ‘lasting bad effects’ from psychological treatment for anxiety or depression ((M. J. Crawford et al., 2016):
- People from Asian ethnic backgrounds are 2.1 times more likely.
- People from Black ethnic backgrounds are 2.5 times more likely.
- People from mixed ethnic backgrounds are 1.5 times more likely.
- People from other ethnic backgrounds are 3.3 times more likely.
- People with severe mental illness (SMI) from Black Caribbean, Black African and Asian ethnic groups stay on psychiatric wards for longer than White patients with SMI (Kapadia et al., 2022).
Additional resources
- The local data pack gives an overview of key data and trends
- Ethnic group, national identity, language and religion summary for Cambridgeshire and Peterborough
- Race/ethnic inequalities in health: moving beyond confusion to focus on fundamental causes
- The NHS Race and Health Observatory report Ethnic Inequalities in Healthcare: A Rapid Evidence Review
- Fact sheet: mental health among young people from racialised communities
- The enduring effects of racism on health: Understanding direct and indirect effects over time
- A literature and evidence review on Racial disparities in mental health
- Making a difference: ethnic inequality and severe mental illness
- Ethnic Inequalities in Mental Health: Promoting Lasting Positive Change
- National Institute of Health Research’s summary of the importance of ethnicity and culture to public mental health
- Cambridgeshire Insight data on population demographics, which includes data on ethnicity from the 2021 Census
- A Constant Battle
- Ethnic health inequalities in later life
- Centre for Mental Health: Pursing Racial Justice in Mental Health
- Ethnic inequalities in improving access to psychological therapies
Gypsy, Roma and Traveller Resources
- Gypsy, Roma and Traveller populations and mental health in the UK: a need for real working together and co-production of services | BJPsych International | Cambridge Core
- Friends Families and Travellers report How to tackle health inequalities in Gpysy, Roma and Traveller communities, a Guide for Health and Care Services.
- Inequalities in Mental Health Care for Gypsy, Roma, and Traveller Communities
Presentations
- Summary slides of the report on Ethnic inequalities in improving access to psychological therapies
Areas for future work
- Map local assets in the community for ethnic minority groups and support building those up
- Are the needs of individuals interpreted by health and mental health care professionals differently depending on patients gender and ethnicity?
- Disaggregation of mental health inequalities by ethnic groups, for children and adults’ mental health services
References
Full list of references is included at the end of this chapter.
