Disability
Disabled people have lower wellbeing scores than non-disabled people, for happiness, worthwhile, and life satisfaction measures. They also report higher levels of anxiety (4.3 out of 10), compared to non-disabled people (2.7 out of 10) (Office for National Statistics, 2019).
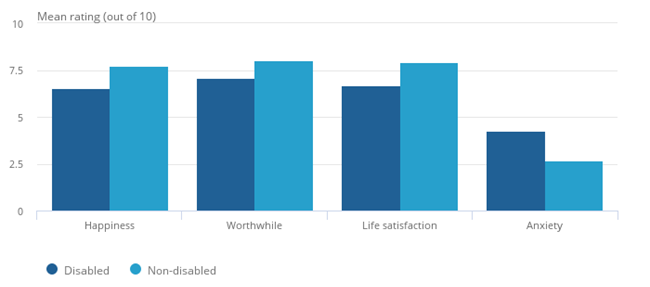
Figure 65: Average wellbeing scores for disabled and non-disabled people, UK, 2018 to 2019. Source: Office for National Statistics
- 40% of Deaf children have mental health conditions, compared to 25% of children without hearing loss (Edwards et al., 2016). 31% of Deaf women and 14% of Deaf men report having depression (Emond et al., 2015).
- Older adults with hearing loss are 2.5 times more likely to develop depression than those without hearing loss (Edwards et al., 2016).
- Around 1 in 3 people with epilepsy have anxiety of depression, over twice the rate in those who do not have epilepsy (Rai et al., 2012).
- Older adults who are visually impaired are more likely to have an anxiety disorder (7.5%) and major depressive disorder (5.4%) compared to their peers (Edwards et al., 2016).
Children and young people with special educational needs and/or disabilities (SEND)
- 16% of children and young people in England have a special education need and/or disability (SEND) (Children and Young People’s Mental Health Coalition & Centre for Mental Health, 2022), ‘a learning difficulty and/or a disability that means they need special health and education support’ (Department for Education, 2023b)
- Children and young people with SEND are more likely to experience social and environmental risk factors for poor mental health, including living in income poverty, living in a household where no adults are in paid work, and parental physical and mental illness (Children and Young People’s Mental Health Coalition & Centre for Mental Health, 2022).
- Half of children and young people (aged 6 to 16) have a probable mental health condition (57%), compared to 13% of those without SEND (Children and Young People’s Mental Health Coalition & Centre for Mental Health, 2022).
- Parents of children and young people with SEND reported that their child showed higher levels of emotional, behavioural and attentional difficulties throughout the pandemic, compared to children and young people without SEND (Children and Young People’s Mental Health Coalition & Centre for Mental Health, 2022).
Local population
Between 14.7 to 19.5% of people in each district of Cambridgeshire and Peterborough have some form of disability (Office for National Statistics, 2023a).
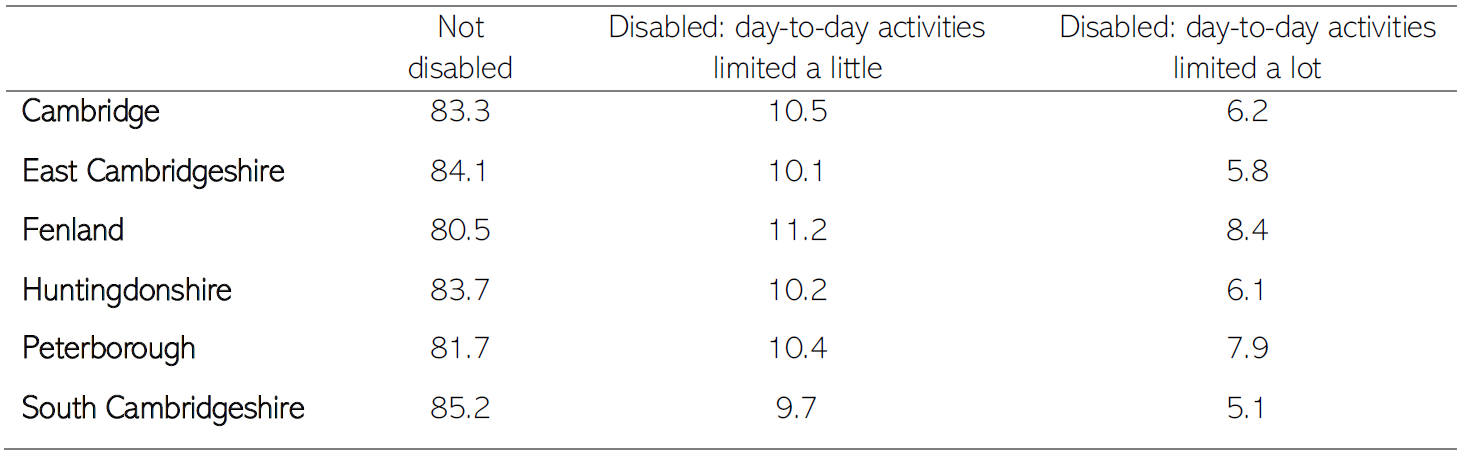
Table 23: Age-standardised proportions of disabled people in C & P. Data source: (Office for National Statistics, 2023a)
National data shows that (Kirk-Wade, 2022):
- 9% of children are disabled, compared to 21% of working age adults and 42% of adults over State Pension age.
- The most common types of disability relate to mobility (46%), stamina, breathing or fatigue (33%), and mental health (29%).
Risk factors for poor mental health
- Disabled people face ‘huge barriers to full inclusion and equality in society’. They face a wide range of inequalities and over a third (36%) have experienced negative attitudes or behaviours from others over the past year (Moss & Frounks, 2022).
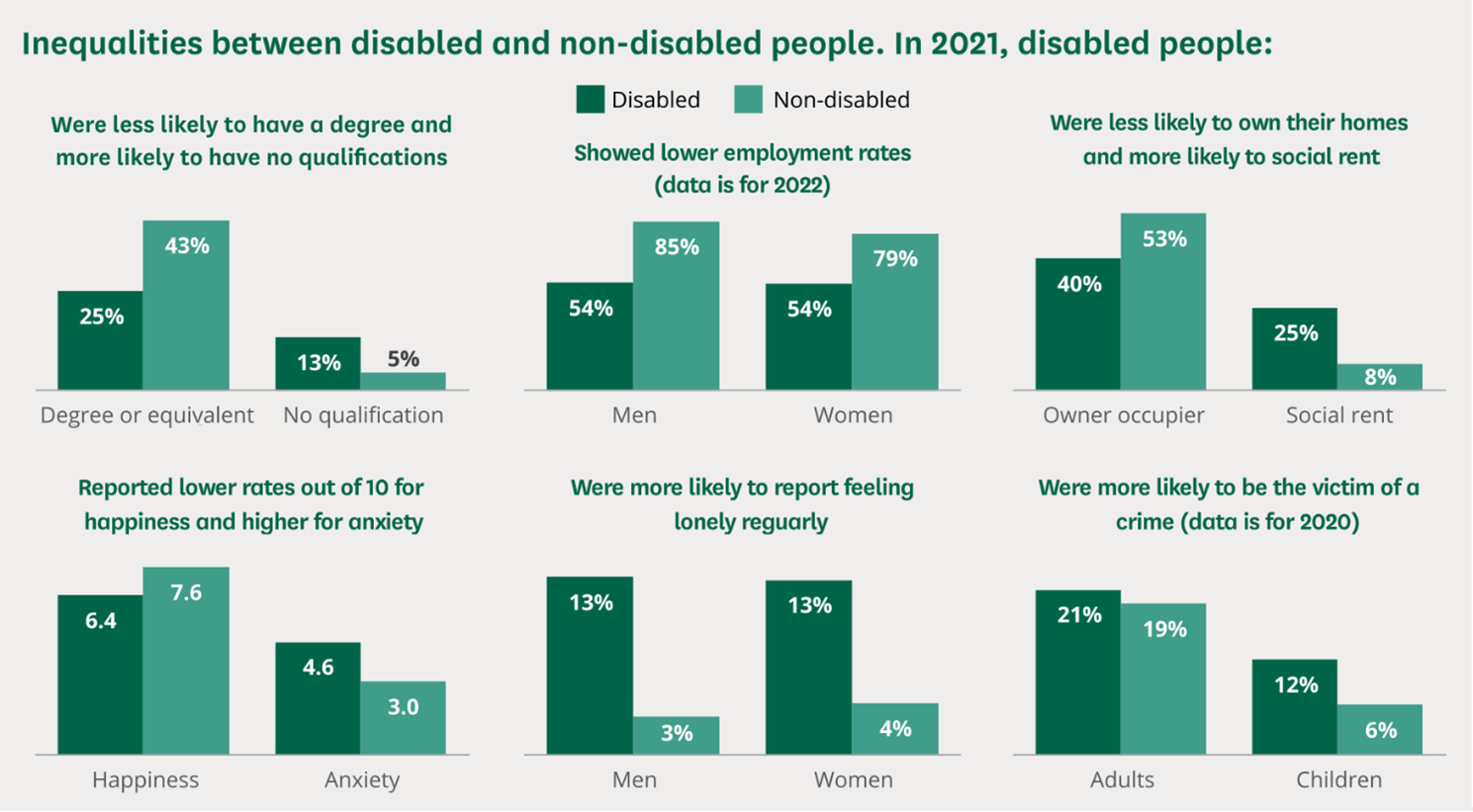
Figure 66: Inequalities between disabled and non-disabled people. Source: House of Commons Library
- Disabled adults face additional costs of £538 a month to afford the same standard of living as a non-disabled people (John et al., 2019).
- Disabled people are at greater risk of experiencing domestic abuse and sexual assault. For example, disabled women are 2.6 times more likely than non-disabled women to experience domestic abuse (Kirk-Wade, 2022).
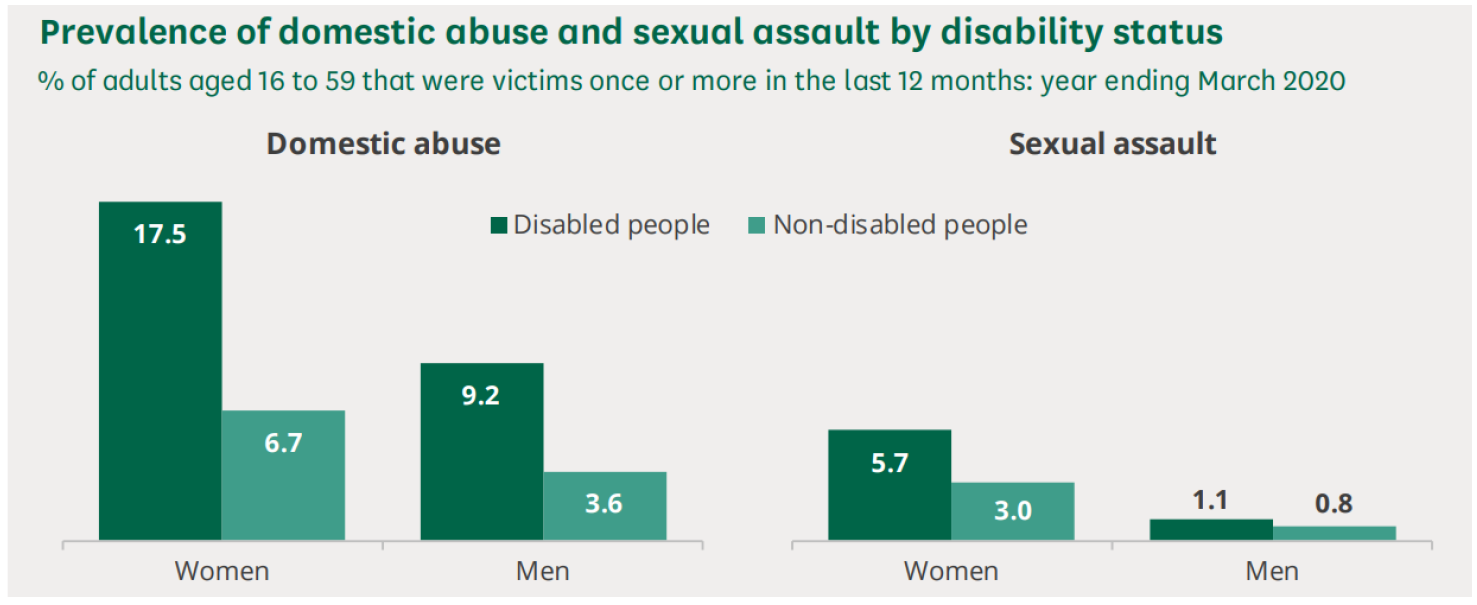
Figure 67: Prevalence of domestic abuse and sexual assault by disability status. Source: House of Commons Library
- The COVID-19 pandemic has had significant impacts on mental health of disabled people, who have reported lower wellbeing than non-disabled people through all stages of the pandemic so far (Kirk-Wade, 2022). In December 2021:
- 50% of disabled people felt that COVID-19 had made their mental health worse.
- 79% of disabled people felt worried or anxious.
- 72% of disabled people were ‘very’ or ‘somewhat’ worried about the effect COVID-19 was having on their life.
Access
- Socioeconomic factors, and the stigma around mental health, are often under-recognised barriers to disabled people accessing mental health care (Morris, 2004). Barriers to accessing mental health services faced by disabled people include:
Structural barriers to accessing mental health support
- Inaccessible and unreliable public transport (Clemente et al., 2022).
- Lack of coordination and communication between physical and mental health services, leading to experiences of fragmented care (Morris, 2004).
- Disabled people are more likely to experience poverty and unemployment, which can make it difficult for people to prioritise mental health or to afford travel costs (Morris, 2004).
Healthcare system barriers to accessing mental health support
- Lack of patient involvement about treatment decisions (Clemente et al., 2022).
- Lack of information provided to carers about the disabled person’s health (Clemente et al., 2022).
- Inaccessible buildings (e.g. lack of wheelchair access, limited disabled parking) (Clemente et al., 2022)
- A lack of interpreters: deaf patients who rely on note-writing with healthcare professionals use fewer preventative healthcare services and receive less counselling than deaf patients with access to interpreters (Fellinger et al., 2012).
- Inaccessible physical environments in inpatient mental health settings (Morris, 2004).
- Difficulties finding accessible talking therapy (Morris, 2004).
- Diagnostic overshadowing (Morris, 2004).
Experience
- People with physical disabilities report that medication required for their physical health is not always available when people are admitted to inpatient mental health wards (Morris, 2004). This can be particularly distressing for people who need regular medication to manage pain (Morris, 2004).
- A lack of understanding around physical disability amongst mental health staff can lead to ‘disempowering attitudes’ (Morris, 2004).
- Many people report not being warned about that impact that psychiatric medications can have on their physical health (Morris, 2004).
- Deaf people report ‘fear, mistrust and frustration’ in mental health services (Fellinger et al., 2012).
- Deaf patients spend twice as long as hearing patients staying in psychiatric inpatient care (Fellinger et al., 2012).
Outcomes
Further work is needed to assess inequalities in mental health outcomes faced by disabled people.
Additional resources
- The local data pack gives an overview of key data and trends
- Joseph Rowntree Foundation report Services for people with physical impairments and mental health support needs
Areas for future work
- Explore inequalities in the prevalence of mental health conditions, and in mental health services, for people with physical disabilities.
References
Full list of references is included at the end of this chapter.
