Victims of crime
The mental health impact of experiencing a crime depends on a range of factors, including but not limited to people’s prior experiences, the type of crime, people’s resources, and stigma. Some of these reponses meet the criteria for mental health conditions, whilst other responses to trauma may not fit this.
This report will focus on two types of crime which have significant impacts on mental health, sexual violence and domestic abuse. These experiences often overlap and are highly prevalent: around a quarter of the general population have some form of experienced physical or sexual abuse (Scott et al., 2015). National research suggests that 4% of people have experienced extensive physical and sexual abuse (Scott et al., 2015). The vast majority (84%) of this group are women (Scott et al., 2015).
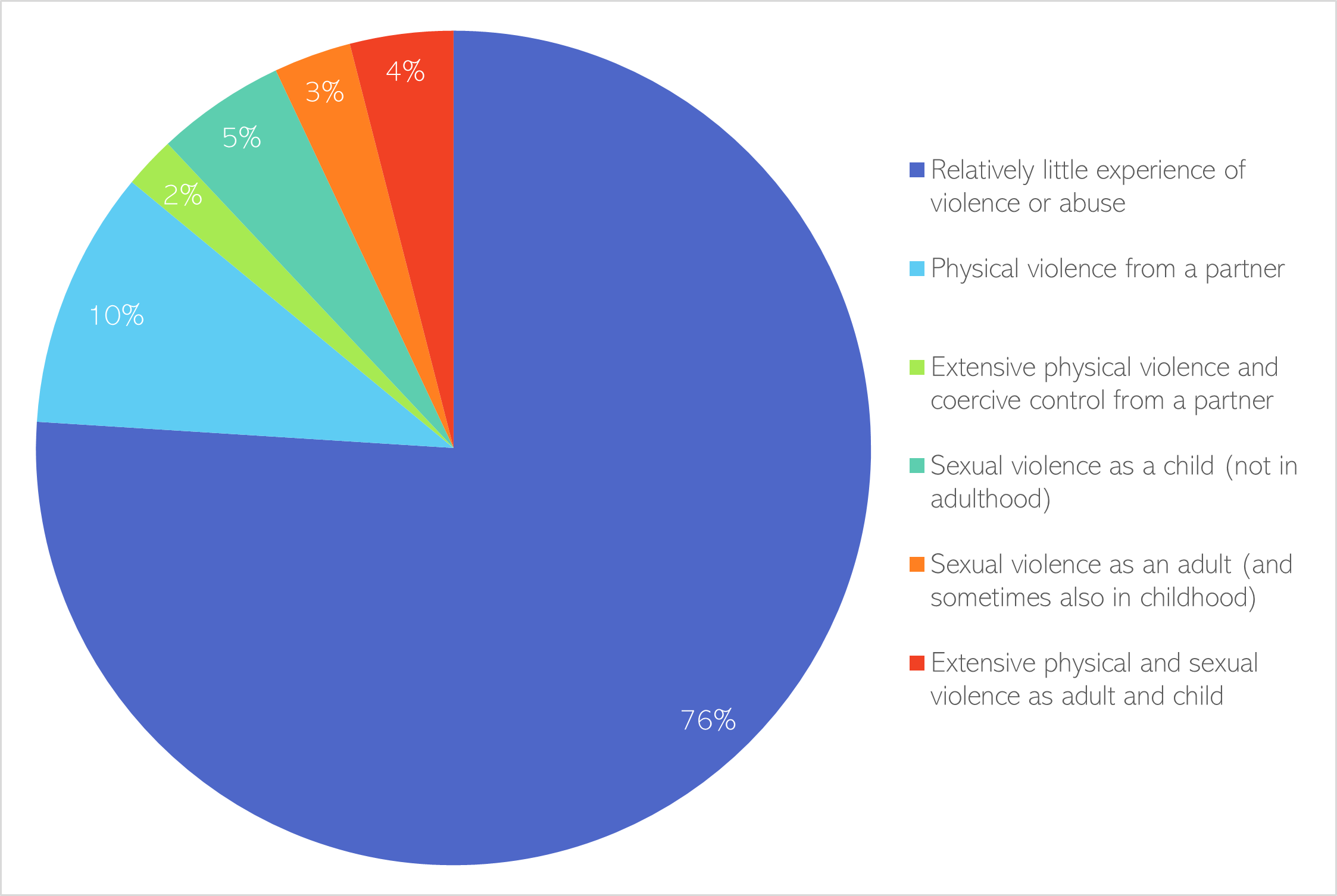
Figure 39: Distribution of violence and abuse in national population. Data source: (Scott et al., 2015)
Sexual violence
Local picture
- An increasing rate of sexual offences is seen in Peterborough and all Cambridgeshire districts, apart from East and South Cambridgeshire (Office for Health Improvement and Disparities, 2023). The rate of sexual offences in Peterborough is higher than the rate in all Cambridgeshire districts and in England.
- These figures are likely to underestimate true levels of sexual violence: national data suggests that fewer than 1 in 6 women and 1 in 5 men who experience rape report it to the police (Office for National Statistics, 2021a).
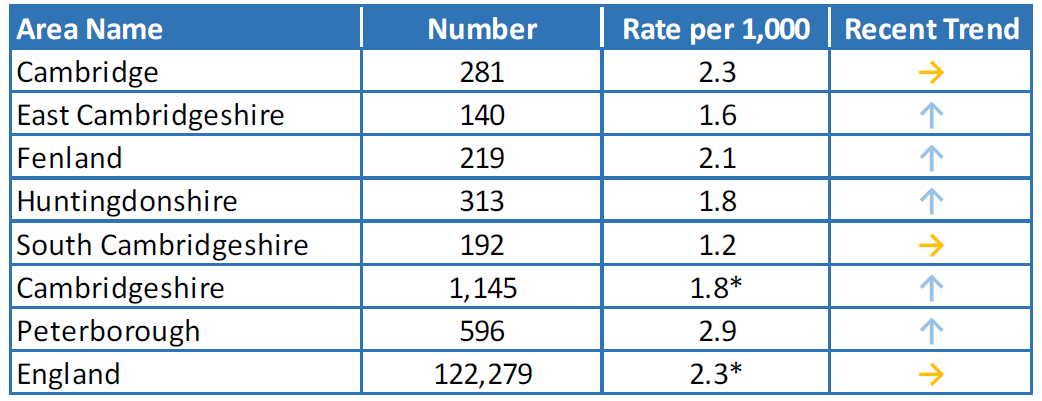
Table 18: Sexual offences per 1,000 population, 2020/21. * indicates where values have been aggregated from all known lower geography values). Data source: Fingertips
- It has been estimated that around 44,000 adults in Cambridgeshire and 10,000 adults in Peterborough are survivors of child sexual abuse.
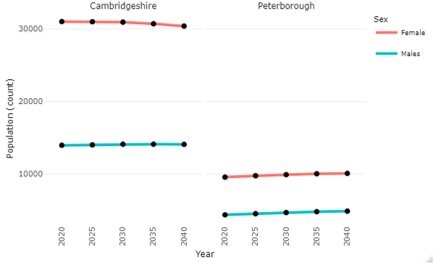
Figure 40: People aged 18-64 predicted to be survivors of childhood sexual abuse. Data source: Projecting Adult Needs and Service Information
Prevalence of mental health conditions
Compared to people with little experience of violence and abuse, people who have experienced extensive sexual and physical violence are as an adult and child are (Scott et al., 2015):
- 5 times more likely to have a common mental health condition.
- 15 times more likely to have multiple mental health conditions.
- 15 times more likely to have attempted suicide.
- 5 times more likely to have self-harmed.
- 12 times more likely to have been an inpatient in a mental health unit.
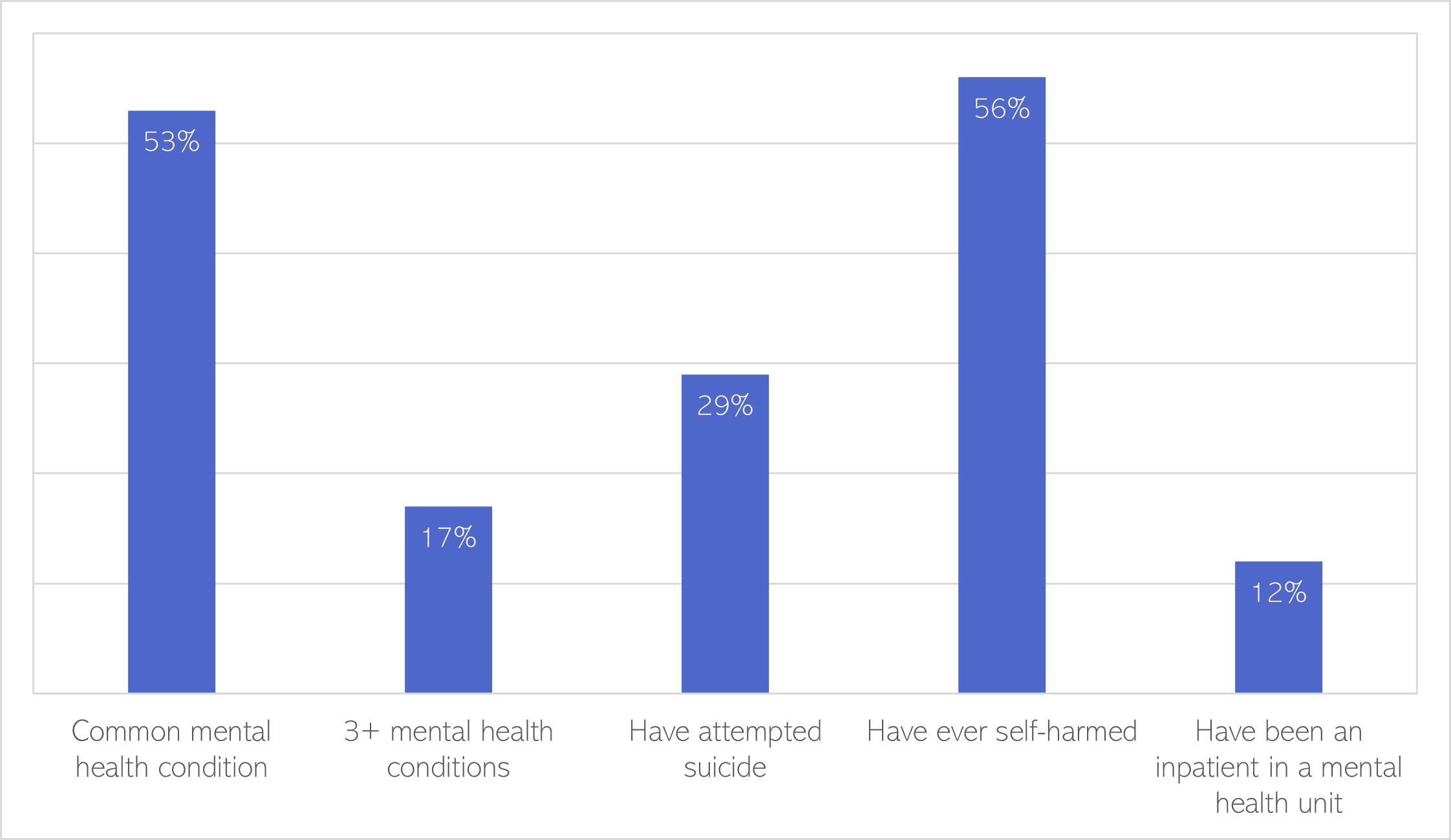
Figure 41: Proportion of people with experience of extensive physical and sexual violence who report the following. Data source: (Scott et al., 2015)
- National data shows that, amongst female survivors of rape, (Office for National Statistics, 2021b):
- 63% report having mental health or emotional problems.
- 50% report having stopped trusting people or having difficulties in their relationships with others.
- 10% have attempted suicide.
- Experiencing sexual assault as a teenager has long term impacts on young people, including on (Clarke et al., 2021):
- Mental health, such as an increased risk of depressive disorders, anxiety and PTSD.
- Physical health.
- Educational outcomes.
- Data from Cambridge Rape Crisis shows that:
- There are currently 125 people receiving trauma-informed counselling and a further 98 requiring therapeutic support with no service available. Of those in the service:
-
- 25% have anxiety and/or depression.
- 23% are struggling with self-harm and/or suicidal thoughts/attempts.
-
- Referrals for counselling services have increased by 183% over the past 2 years (Cambridgeshire and Peterborough Domestic Abuse and Sexual Violence Partnership, 2022).
- There are currently 125 people receiving trauma-informed counselling and a further 98 requiring therapeutic support with no service available. Of those in the service:
Access and experience
Further work is needed locally to understand the experience of survivors of sexual violence in accessing mental health support. Stakeholders report difficulties in accessing mainstream services because of complexity of need:
- Survivors often feel powerless as a result of experiencing sexual violence, and this can be emulated by healthcare professionals.
- Some people end up being ‘bounced around’ services,
- Some people may not want a mental health diagnosis, but to instead be recognised as survivors of sexual violence. This will be looked at in more detail in Chapter 7.
Outcomes
People with experiences of child sexual/physical abuse have lower recovery rates in NHS Talking Therapies (previously known as IAPT) (Verbist et al., 2021).
Domestic abuse
Local population
There was a peak in referrals to Cambridgeshire and Peterborough Independent Domestic Violence Advisor service in the first quarter of 2021/22, though rates have since reduced (Domestic Abuse Team, 2022). This service supports medium-high risk victims of domestic abuse.
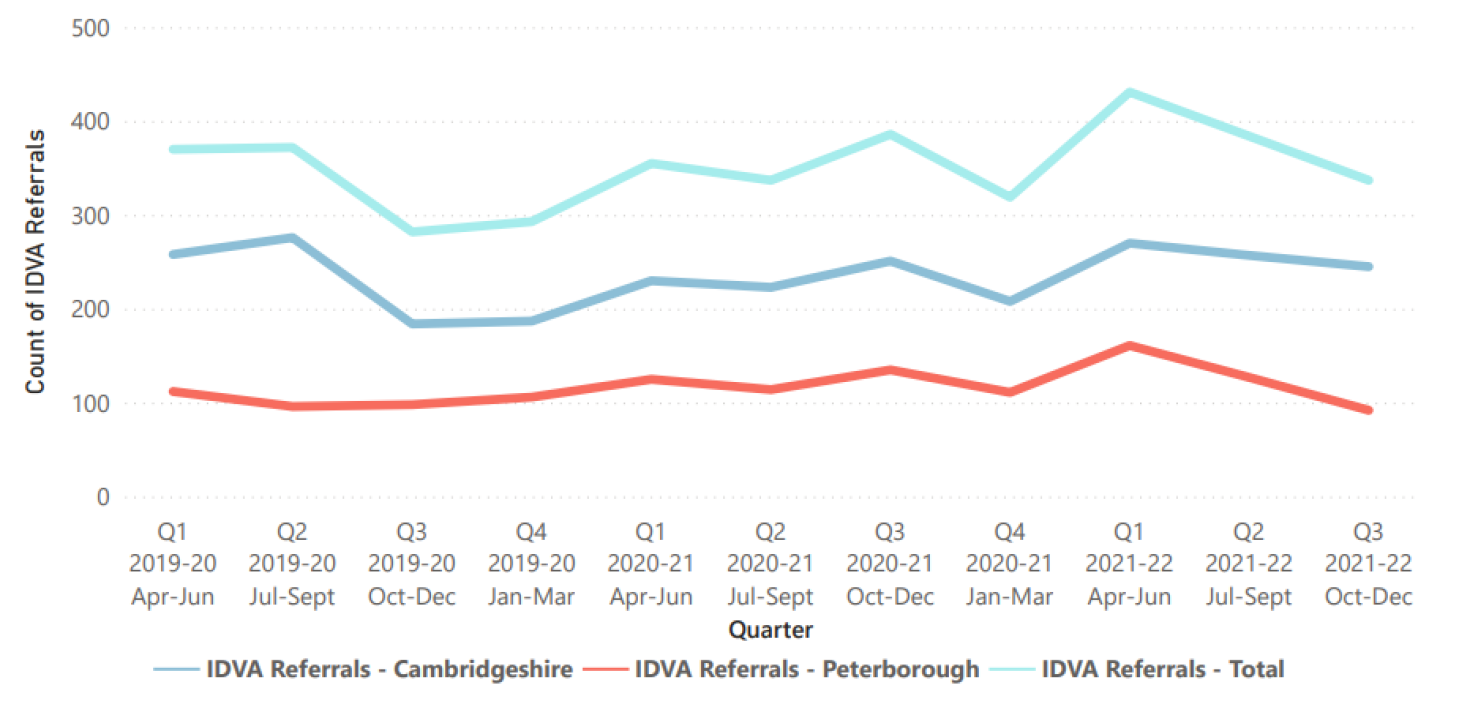
Figure 42: Quarterly IDVA Referrals Counts in Cambridgeshire and Peterborough. Source: Domestic Abuse Team – Quarterly DA Performance Report, Cambridgeshire and Peterborough (2019-2021)
- Past needs assessments show that domestic abuse cases make up a high proportion of crimes recorded in Cambridgeshire (Cambridgeshire County Council, 2020).
Summary: Victims, Suspects and Offenders Needs Assessment 2019/20 (Cambridgeshire County Council, 2020)
Markers relating to victim vulnerability were analysed in 2019, with a total of 8,993 unique victims having at least one of the following 5 ‘vulnerability markers’ within the police recording system.
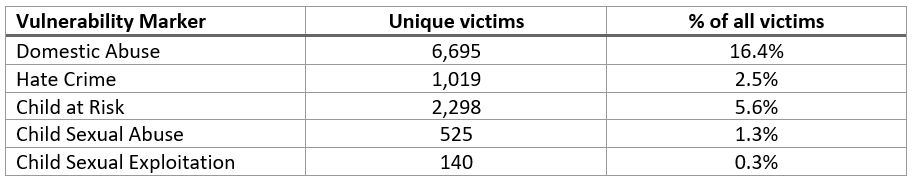
Table 19: Number of victims who experienced a crime with one of these 5 vulnerability markers as recorded by Cambridgeshire Constabulary in 2019.
- Domestic abuse victims were more likely to be repeat victims, female and aged 30-39 at the time of the offence.
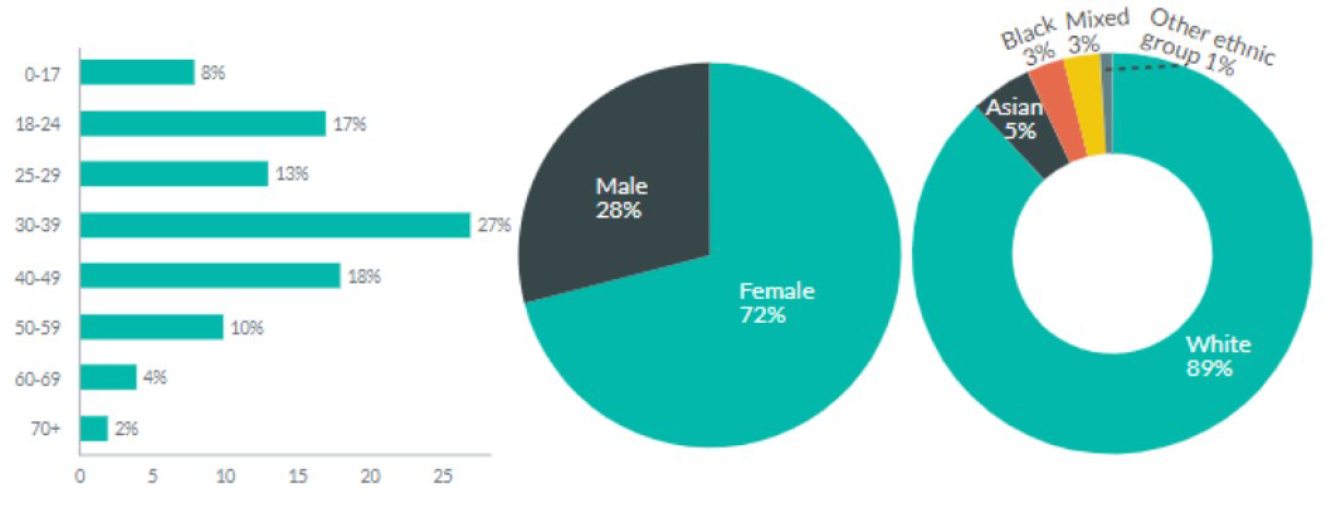
Figure 43: Demographic breakdown, where known, for those victims with a vulnerability marker for domestic abuse
- However, domestic abuse is a ‘hidden crime’ that often goes underreported: the Crime Survey for England and Wales estimates that 5.7% of adults (aged between 16 and 59) experienced domestic abuse in the year ending March 2022 (ONS, 2020).
- National data also suggests that a significant proportion of children and young people live in households where domestic violence is taking place:
- One survey found that 12.0% of children under 12, and 18.4% of young people aged 11 to 17, have ever witnessed domestic abuse or threatening behaviour at home (Moroz, 2021).
- 62% of children and young people living in households where domestic abuse is taking place have been directly harmed the perpetrator of the abuse (Moroz, 2021).
Prevalence of mental health conditions
National research estimates that around 30 to 60% of women with mental health problems have experienced domestic abuse (Howard et al., 2010). Domestic abuse has a range of harmful impacts on health, including increasing risk of mental health conditions and substance use.
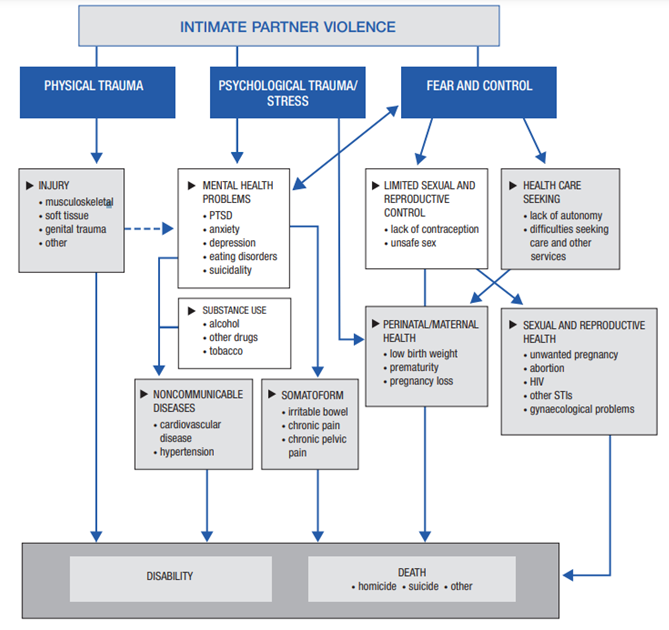
Figure 44: The health impacts of intimate partner violence. Image source: World Health Organisation
- People who have experienced abuse from a partner within their lifetime are, in the past year, (McManus et al., 2022):
- 2.8 times more likely to have attempted suicide.
- 2.2 times more likely to have self-harmed.
- 1.9 times more likely to have suicidal thoughts.
- One survey of survivors of psychological/emotional abuse found that (Safe Lives, 2019):
- 90% reported low self-esteem.
- 88% felt emotionally withdrawn or shut down.
- 84% felt lonely and isolated.
- 47% reported having suicidal thoughts.
- In the most recent national analysis of domestic homicide reviews (reviews into deaths of adults which may have resulted from violence, abuse or neglect), it was found that around a third of both victims and perpetrators had a mental health vulnerability (Home Office, 2022).
- The health impacts of domestic abuse can be long-term, with one study estimating the increased lifetime healthcare costs of experiencing domestic abuse from a partner being over £26,000 (William et al., 2002). Similarly, there are high healthcare costs for people who experience a combination of poor mental health, substance abuse and domestic abuse.
- Exposure to or witnessing domestic abuse is an adverse childhood experience and can have a significant detrimental impact on children and young people (Moroz, 2021). This includes impacts on emotional and psychological wellbeing, sense of safety and trust in others, relationships with family and friends, behaviour and school performance.
Access
- A 2010 national review of mental health services found professionals did not routinely enquire about domestic abuse, and that as a result, domestic abuse was under-recognised in mental health services (Trevillion et al., 2016). Barriers to people disclosing abuse included (Trevillion et al., 2016):
- Individuals not recognising behaviours they had experienced as abusive.
- People feeling shame around their experiences.
- Fear that they would not be believed, or that disclosing would have negative consequences (such as the involvement of social services, escalation of violence, or threats to immigration status).
- Being isolated from family and friends by perpetrators.
- Professionals focusing on diagnosing and treating mental health conditions, and ignoring wider social causes of poor mental health.
- Barriers to support for children and young people who witness domestic abuse include (Moroz, 2021):
- Lack of insight into the impact that witnessing domestic abuse have on children and young people.
- The timing and method of support provision.
- Concerns around privacy and external judgement, such as fear about the consequences if the perpetrator became aware.
Experience
- Nationally, people report low levels of satisfaction with the response of mental health services to domestic abuse (Trevillion et al., 2016).
- A review of people’s experiences of disclosing experiences of domestic abuse in mental health services found that professionals rarely gave responses that prioritised patient safety (Trevillion et al., 2016).
- Many mental health professionals lack knowledge and confidence about the best ways to respond to disclosures of domestic violence (Trevillion et al., 2016).
Outcomes
More work needs to be done to explore the mental health outcomes of people who have experienced domestic abuse, at both a national and local level.
Additional resources
- The local data pack gives an overview of key data and trends
- Past local Needs Assessments: Victims, Suspects and Offenders 2019/20; Violence Against Women and Girls (VAWG) Needs Assessment 2017
- Violence, abuse and mental health in England: Population Patterns
- Responding to violence against women and children – the role of the NHS
- Victim Support’s report Restoring trust Children witnessing domestic abuse: learnings for support services
References
Full list of references is included at the end of this chapter.
