Socioeconomic deprivation
The local picture of deprivation, and the link between deprivation and mental health, is covered in Chapter One of this needs assessment.
Access
Structural barriers to accessing mental health support
- People living in more deprived areas are more likely to have inflexible jobs, in which they are unable to take time out to access medical care during regular working hours. Having an inflexible job is associated with reduced access to GPs and a lower health-related quality of life (Moss et al., 2022).
- The cost-of-living crisis is preventing people being able to access healthcare. For example, a survey in December 2022 found that 11% of people had avoided booking NHS appointments due to the associated costs, such as the cost of internet use or of making a phone call (Healthwatch, 2023). This is a sharp increase from 7% of people in October 2022.
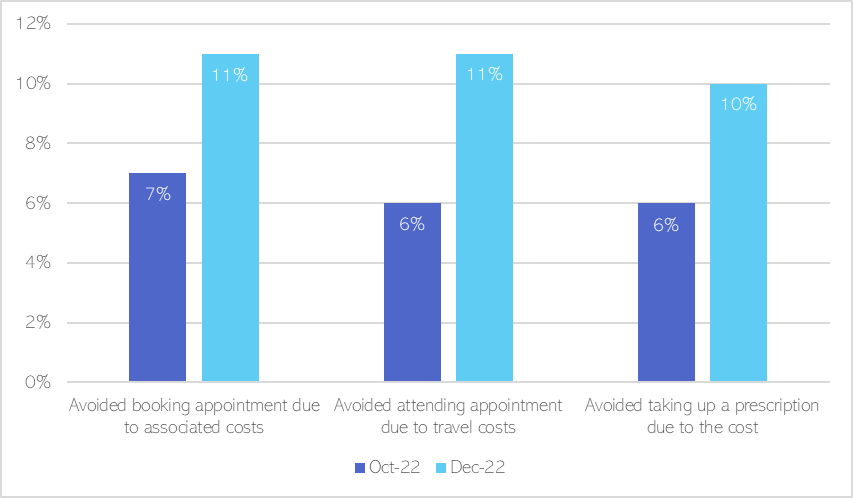
Figure 9: Increase in the proportion of people avoiding NHS healthcare due to associated costs of making bookings, travel and prescriptions, from October 2022 to December 2022. Data source: (Healthwatch, 2023)
- People in manual jobs face barriers to accessing digital healthcare: people in semi-skilled, or unskilled manual occupations, and those who are unemployed, are 7 times more likely to lack internet access at home, compared to those in managerial, administrative, professional occupations (Ofcom, 2022).
Healthcare system/individual barriers to accessing mental health support
- The inverse care law is present in Talking Therapies (previously known as IAPT): in more deprived areas, there is a greater mental health need, and a larger number of people are referred to Talking Therapies. However, there is no relationship between deprivation and number of people who receive care through this service (Delgadillo et al., 2016).
- A small study found that people living in more deprived areas who are referred to CBT or counselling were less likely to opt-in to therapy or attend their first appointment (Grant et al., 2012).
Experience
People living in the most deprived neighbourhoods in Cambridgeshire and Peterborough are 3.5 times more likely to be detained under the Mental Health Act than those living in the least deprived areas (NHS Digital, 2022).
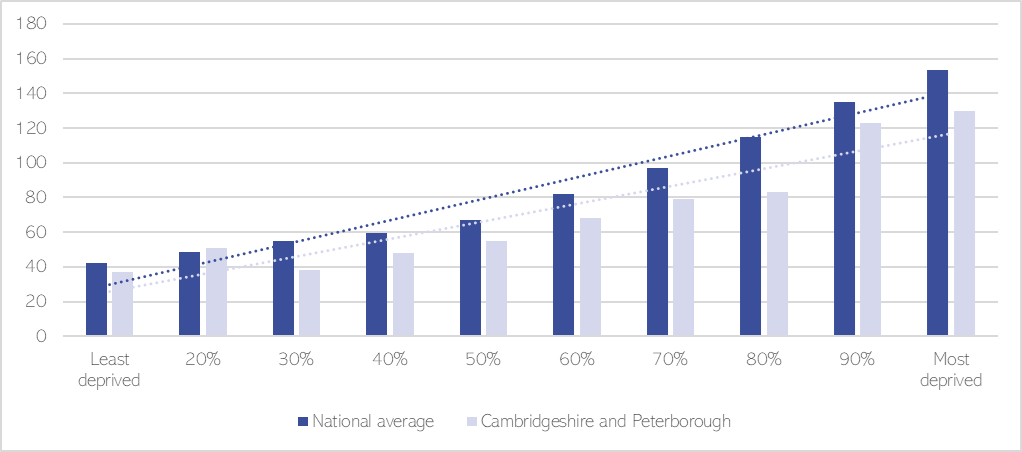
Figure 10: Rates of detention under the Mental Health Act per 100,000 of the population in 2021/22, by deprivation level (IMD) in C & P. Data source: (NHS Digital, 2022)
General practices in the most deprived areas of C & P have fewer GPs and greater numbers of nurses, compared to the least deprived areas (Ford, 2020).
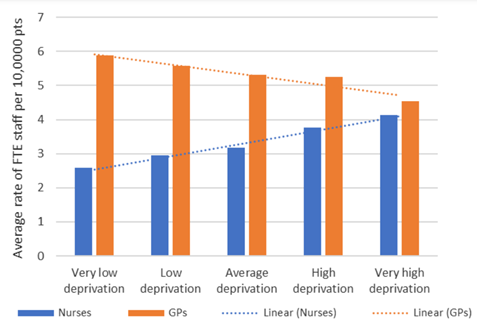
Figure 11: Primary care GP and nurse inequalities in C & P in December 2019. Source: Ford 2019
People living in more deprived areas have shorter GP consultations (Gopfert et al., 2021). For example, people living the most deprived 20% of neighbourhoods, who have both physical and mental health conditions, have a similar consultation lengths as those from the least deprived 20% of neighbourhoods who do not have multiple health conditions.
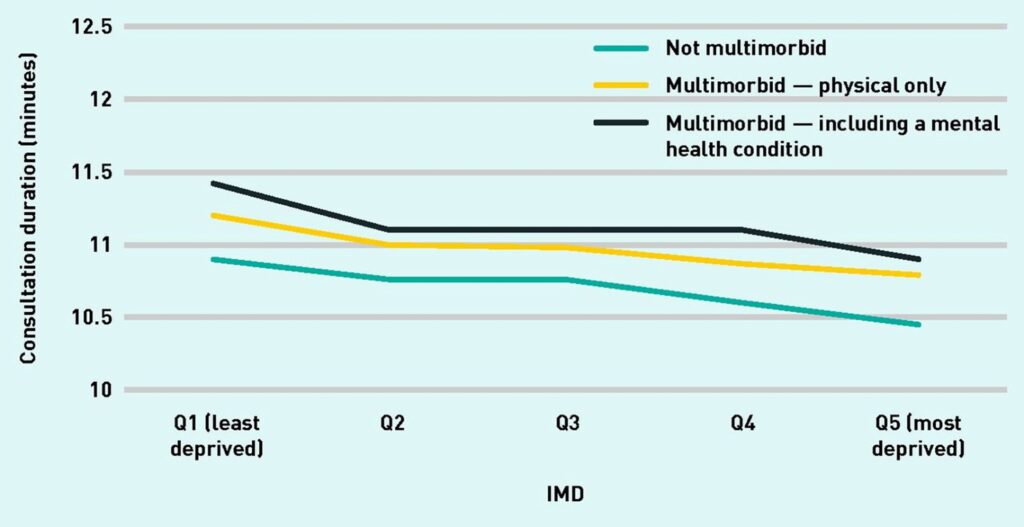
Figure 12: GP consultation by quintile (Q) of Index of Multiple Deprivation (IMD) and multimorbidity type. ‘Multimorbidity – physical only’ was defined as 2+ physical conditions and no mental health conditions; whilst ‘multimorbid — including a mental health condition’ was defined as 2+ conditions, including at least 1 mental health condition. Source: Gopfert et al. 2021
Evidence suggests that there is no association between deprivation and dropout rates for psychological therapies for people with common mental health conditions (N. Firth et al., 2022).
Outcomes
National data shows that people living in the most deprived areas are more likely to die by suicide (Windsor-Shellard, 2020). The association with deprivation is only seen in people of working age; and is largest for men aged between 35 and 55 (Windsor-Shellard, 2020).
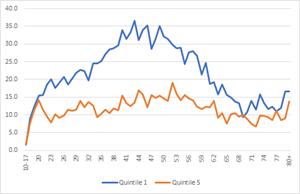
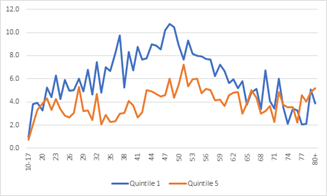
Figure 13: Age-specific suicide rates for males (top) and females (bottom) from the highest and lowest IMD quintile, England, 2010 to 2019 registrations combined. Source: (Windsor-Shellard, 2020)
Recovery rates from mental health conditions are lower in more deprived neighbourhoods (Delgadillo et al., 2016). For example, people living in more deprived areas have poorer outcomes after receiving treatment for depression and anxiety through Talking Therapies. They tend to require more sessions of therapy in order to benefit (Finegan et al., 2020).
Additional resources
-
- The local data pack gives an overview of key data and trends
- NIHR summary of why deprivation is important to public mental health
- The Health Foundation evidence hub on health inequalities
- Centre for Mental Health briefing on Poverty, economic inequality and mental health
- Further local data on deprivation
- Kings Fund: Illustrating the relationship between poverty and NHS services
- Poverty-Proofing-Toolkit.pdf
References
Full list of references is included at the end of this chapter.
