Adult offenders
- There is a high level of mental health need across the criminal justice system:
- 29% of people in police custody have a mental health condition (Criminal Justice Joint Inspectorate, 2021a).
- 38% of people on probation supervision have a recorded mental health condition (Criminal Justice Joint Inspection & Care Quality Commission, 2021).
- 71% of women and 47% of men in adult prisons report having mental health problems (Prison Reform Trust, 2022).

Figure 33: Mental health need across the criminal justice system. Data source:(Criminal Justice Joint Inspectorate, 2021a; Prison Reform Trust, 2022)
Local population
- The total number of people in prison in Cambridgeshire and Peterborough has been relatively stable over the past 5 years.
- HMP Littlehey is a category C men’s prison
- HMP Peterborough is a category B dual purpose prison for men and women
- HMP Whitemoor is a category A (high security) men’s prison
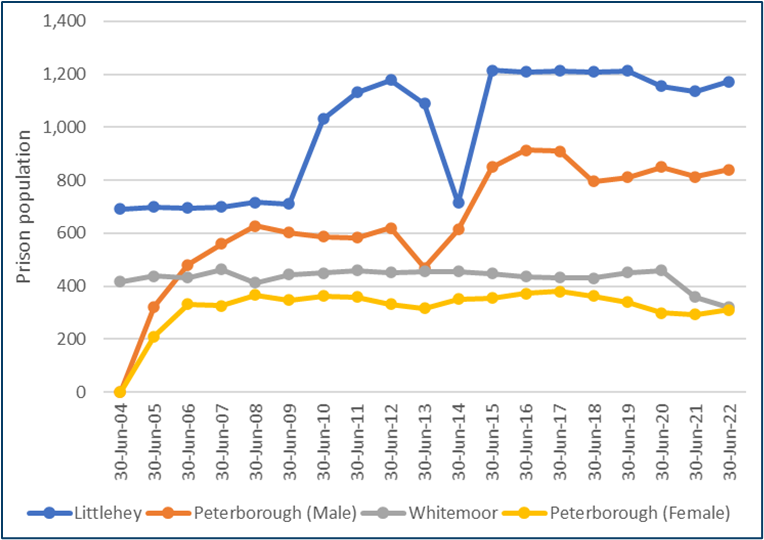
Figure 32: Total number of people in prison in C & P. Data source: (Ministry of Justice, 2022)
Mental health need
Amongst people in prison, studies suggest that that most common mental health conditions are personality disorders and neurotic disorders such as depression (Singleton et al., 1998).
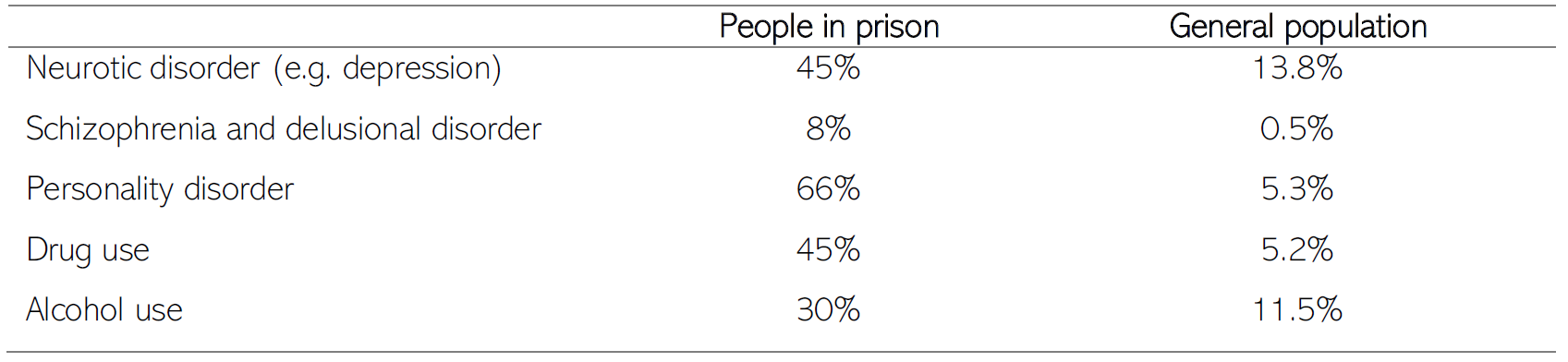
Table 16: Rates of mental health and harmful substance use amongst people in prison and the general population. Data source: (Singleton et al., 1998)
- The mental health conditions of people in prison tend to be more severe and complex than those in the general population; with many people having had traumatic experiences and histories of being in care (Durcan, 2014).
- Alongside being at high risk of having mental health conditions, people in prison often use substances and have poor physical health (Public Health England, 2019b). Many people develop substance use issues within the criminal justice system: one 2018 survey of UK prison found that 30% of people had begun drug use since entering prison (HM Chief Inspector of Prisons, 2019).
- When people are detained, this can exacerbate poor mental health and increase risk of self-harm and suicide (NHS England, 2016b).
- Women in prison have a higher prevalence of self-harm, suicide attempts, psychosis, anxiety and depression than both women in the general population and men in prison (Department of Health & Social Care, 2018).
Probation
- There had been relatively little research into the mental health of people under probation service supervision (Richards, 2020). However, there appears to be high levels of need, with one study of people in contact with probation services finding that (Richards, 2020):
- 39% had a current mental health condition, of whom 72% had co-occurring substance use.
- 49% had ever had a mental health condition.
- 27% had some form of anxiety disorder (such as PTSD, OCD or generalised anxiety).
- 5% had an eating disorder.
- Various surveys have found that between 43 to 55% of people under probation service supervision have harmful levels of alcohol use (Richards, 2020).
- Unmet health and social needs can prevent people from being able to engage with probation services (Richards, 2020).
Summary: What next for Probation? Findings and recommendations from our Lived Experience Inquiry into Probation (Mullen et al., 2021)
A national report based on work with people with lived experience of probation highlights that:
-
- Probation practitioners can be vital in helping people to address the root causes of their offending; and people highly value their support when accessing mental health and housing services.
- Being linked into community-based services, which provide social interaction and the chance to build skills, were highlighted as being particularly important to improving people’s mental health.
- However, people reported that probation practitioners are often unable to offer the right support to people on probation, sometimes due to a lack of time or resources.
- The fear of being recalled to prison often reduced people’s willingness to discuss issues in their lives (such as mental health conditions or having been a victim of a crime).
Liaison and diversion services
Liaison and diversion (L&D) services aim to improve health outcomes and reduce re-offending, by providing early intervention for vulnerable people as soon as they come in contact with the criminal justice system.
- One large scale study found that people who use L&D services whilst in police custody are (Kane et al., 2020):
- Less likely to re-offend, regardless of the offence type.
- Less likely to undergo compulsory admission to mental health services.
- L&D services can support courts to make informed sentencing decisions, including identifying where Mental Health Treatment Requirements (MHTRs) are appropriate:
- MHTRs were introduced in 2005, so that offenders with mental health conditions can be given community orders with mental health treatment, instead of being imprisoned.
- In 2019, just 781 MHTRs were put in place nationally under community orders or suspended community orders (Ministry of Justice, 2020).
- MHRTs are associated with reductions in reoffending, of around 3.5% when used as part of a community order, and 5% when used as part of a suspended sentence order (Ministry of Justice, 2020).
Local mental health need in adult offenders
- Recent data from probation services in Cambridgeshire and Peterborough shows that:
- There have been small numbers of Alcohol Abstinence and Monitoring Requirements given each month, since their introduction in March 2021.
- There has been a recent increase in the number of Drug Rehabilitation Requirements.
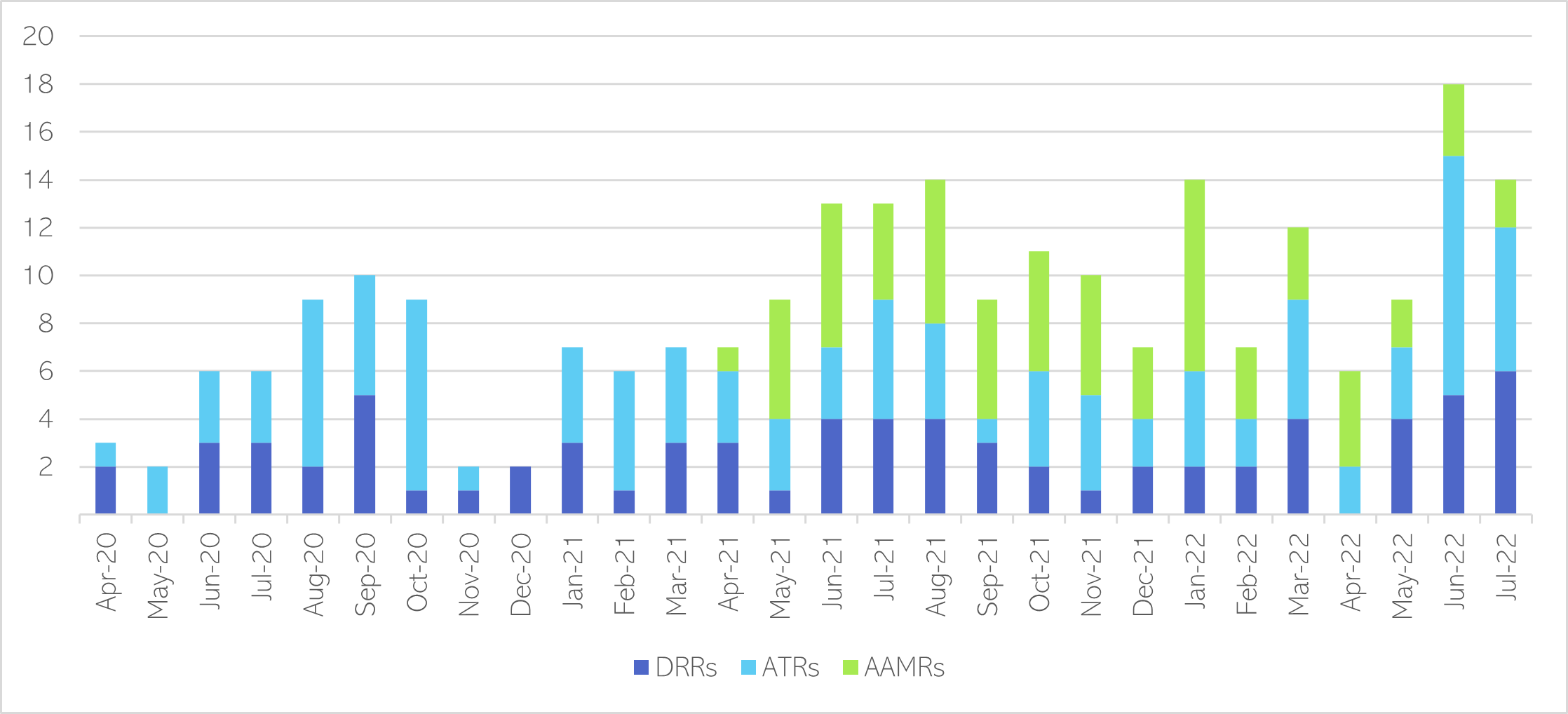
Figure 34: Number of Drug Rehabilitation Requirements (DRRs), Alcohol Treatment Requirements (ATRs) and Alcohol Abstinence and Monitoring Requirements (AAMRs) ordered by C & P courts each month, from April 2020 – July 2022.
Findings from previous local needs assessments are summarised below:
Summary: Victims, Suspects and Offenders Needs Assessment 2019/20 (Cambridgeshire County Council, 2020)
-
-
- This report for Cambridgeshire and Peterborough highlighted most individuals within the criminal justice system have complex and multiple needs:
- 73% of adults assessed by BeNCH Community Rehabilitation Company had 4+ needs.
- 87% for adults assessed by the National Probation Service had 4+ needs.
- One the key conclusions of the report was that accommodation remains a key need for offenders; and that a lack of accommodation or inappropriate accommodation is an important driver of re-offending.
- Education, training and employment, mental health and substance use were also highlighted as ‘substantial concerns’.
- This report for Cambridgeshire and Peterborough highlighted most individuals within the criminal justice system have complex and multiple needs:
-
Summary: Offenders Needs Assessment 2017 (Cambridgeshire County Council, 2017)
-
- This report highlighted a high level of recorded mental health need in the local criminal justice system.
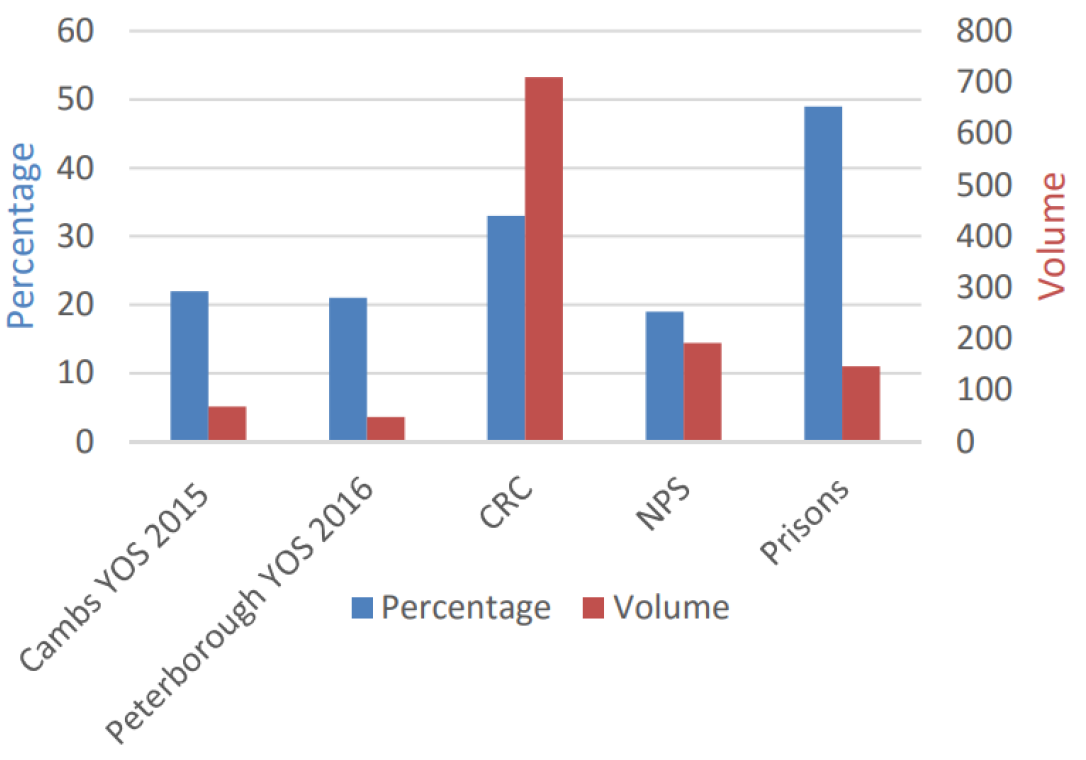
- Figure 35: Volume and percentage of mental health need in local YOS (Youth Offender Service), CRC (Community Rehabilitation Company), NPS (National Probation Service) and prisons. Image source: Offenders Needs Assessment
- This report highlighted the following ‘gaps’:
- A high percentage and volume of individuals in contact with the criminal justice system have a mental health condition, which are often linked with drug and alcohol use and homelessness.
- The mental health system has limited capacity to meet these needs.
- The report also highlighted the following focus areas for future work:
- Comprehensive service mapping of mental health services which includes offender aspects.
- Working with partners to understanding and address frequent attenders across the system.
- Further work with partners to help those with complex needs such as mental health, substance use and homelessness.
Risk factors for poor mental health
‘Record high numbers of self-inflicted deaths and incidents of self-harm in prisons are a damning indictment of the current state of the mental health of those in prison and the prison environment overall’ (The Committee of Public Accounts, 2017)
- There is a very high prevalence of adverse childhood experiences and other psychological traumas amongst people in prison (Durcan, 2020).
- Poor conditions in prison can make it difficult for people in prison to manage their mental health. This includes bullying, violence and social isolation.
- The earlier stages of the COVID-19 pandemic saw the majority of people in prison confined to their cells for 23 hours a day, 7 days a week, without any visits from family, friends or partners (Justice Committee, 2021). The HM Inspectorate of Prisons states this had a ‘profound’ impact on mental health, with ‘hopelessness and helplessness becoming engrained’ in many people (Aspinall & Watters, 2010; HM Inspectorate of Prisons, 2021).
- The 2007 Corston report urgently highlighted the need for ‘better ways to keep out of prison those women who pose no threat to society’ and highlights that ‘prison is not the right place for many women… [and that] they need help and caring, therapeutic environments to assist them rebuild their lives’ (Corston, 2007).
- Older people in prison can age prematurely due to their living conditions and tend to have high rates of physical health problems (Durcan, 2020).
- Upon leaving prison, many people are at risk of homelessness (Richards, 2020). Estimate levels of risk vary, with national research from Homeless Link finding that 15% of men and 13% of women leaving prison have ‘no fixed abode’ as their accommodations status (Richards, 2020).
Access
‘Government does not have reliable or up-to-date measure of the number of people in prison who have mental health problems and existing screening procedures are insufficient to adequately identify those who need support and treatment’ (The Committee of Public Accounts, 2017)
Accessible and effective mental healthcare is an essential part ensuring people released from prison can successfully rebuild their lives in the community (The Committee of Public Accounts, 2017).
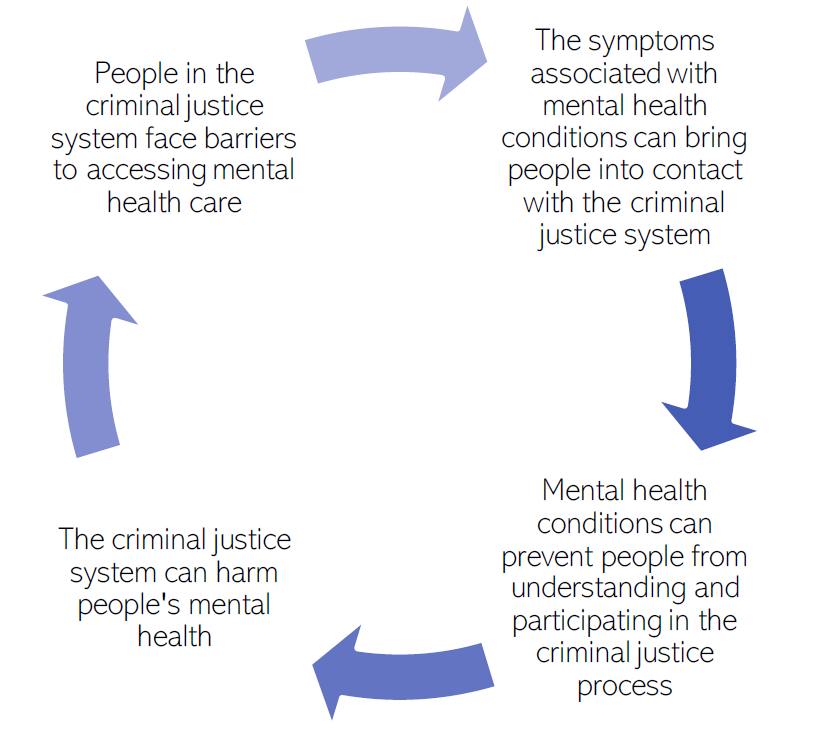
Figure 36: The links between mental health and the criminal justice system. Adapted from: (Criminal Justice Joint Inspection & Care Quality Commission, 2021)
Barriers to accessing mental health services faced by adults in contact with the criminal justice system include:
Structural barriers to accessing mental health support
- People in prison miss around 1 in 7 doctor’s appointments, most commonly due to a lack of staff to escort them (The Committee of Public Accounts, 2017).
- COVID-19 restrictions exacerbated difficulties accessing mental health treatment, as group-based therapies were cancelled, and no alternative support was provided (Justice Committee, 2021).
Healthcare system barriers to accessing mental health support
- The mental health needs of people in contact with the criminal justice system are often not recognised:
- 1 in 12 people do not get the health screening they should receive within 24 hours after entering prison (Justice Committee, 2021).
- People from ethnic minority backgrounds are less likely to be identified as having learning difficulties or mental health problems upon arrival at prison (Justice Committee, 2021).
- Mental health conditions often identified late in the parole process; which can cause delays and make it difficult for staff provide support which allows people to meaningfully engage in parole reviews (Justice Committee, 2021).
- There is no common definition of mental health used across the criminal justice system, hence individuals’ needs may be missed as they pass between agencies (Criminal Justice Joint Inspectorate, 2021a).
- Nationally, people report experiencing ‘enormous difficulties’ in receiving medications for mental health conditions after arriving in prison (Durcan, 2020).
- The NHS target for acutely ill people in prison to be transferred to inpatient mental health services is 14 days. However, due to a shortage of secure mental health beds, average transfer times are very much longer (Woods et al., 2020):
- For example, the average wait for a high security bed is 157 days.
- As a result of these delays, acutely ill patients are segregated in prisons instead of being treated in hospital.
Experience
People with experience of the criminal justice system: ‘experience stigma and discrimination and struggle to get the right help at the right time. Such issues are exacerbated by mistrust of healthcare professionals, transient lifestyles, negative attitudes amongst healthcare staff towards offenders, problems with interagency communication and inflexible or insufficient service provision so their access to healthcare is often less than they need. Many individuals are not registered with a GP and most only access healthcare in a crisis’ (NHS England, 2016b)
- Criminal justice and healthcare professionals highlight concerns about the ability of mental health systems to support people in contact with the criminal justice system who have complex needs (Durcan, 2014). They report that there is an unmet need for holistic support for people with multiple and complex needs, who would benefit from services that extend beyond mental health care, to wider services such as housing and benefits advice (Durcan, 2014).
- People entering prison on remand and on short sentences tend to have the highest levels of mental health need, yet experience particularly poor continuity of care (Durcan, 2020).
- There is limited research on the experiences of people from ethnic minority groups in prison, although one study shows that they are less likely to have their mental health needs met (McKenzie et al., 2019).
Outcomes
National rates of suicide and self-harm in prisons have risen significantly since 2011 (The Committee of Public Accounts, 2017).
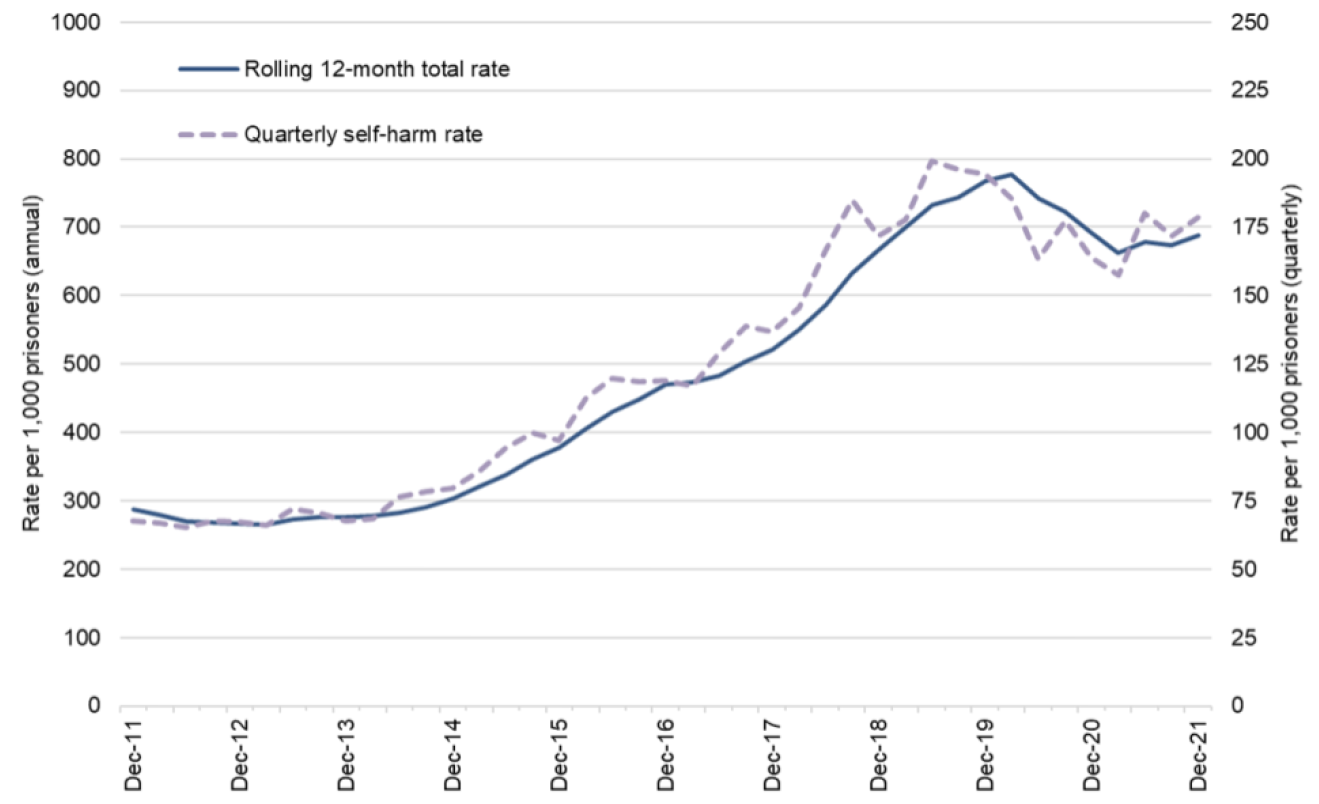
Figure 37: National 12-month rolling rate, and quarterly rate, of self-harm incidents per 1,000 people in prison. Data source: (Ministry of Justice & HM Prison & Probation Service, 2022)
People who have been released from prison are at a much higher risk of dying from a drug-related cause, or by suicide, than the general population (NHS England, 2016b).
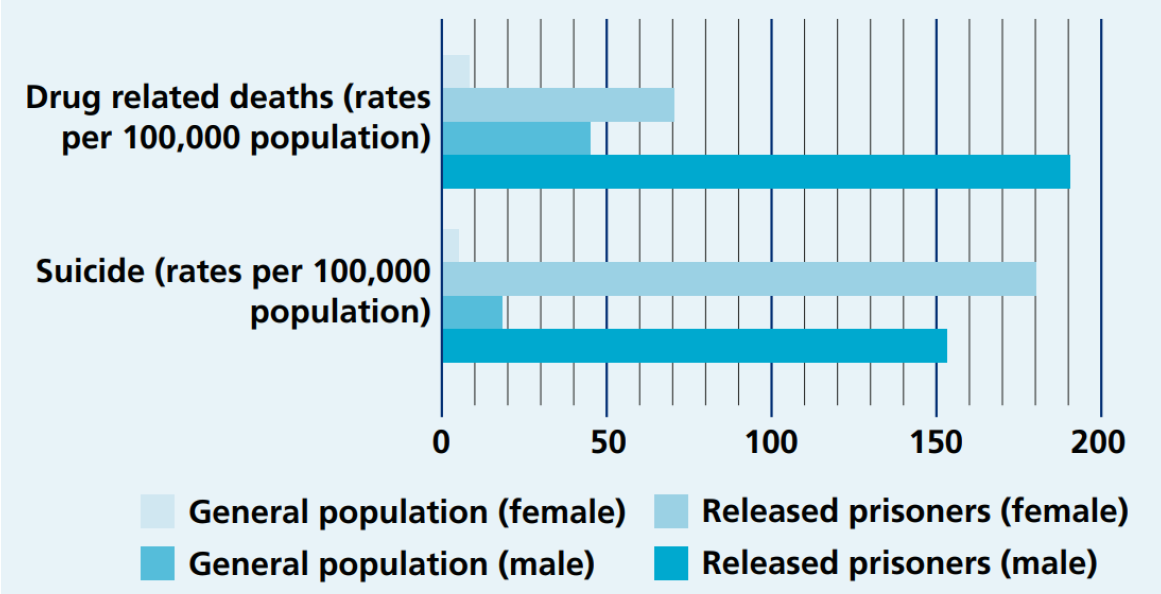
Figure 38: National drug-related deaths and suicide rates among people who have been released with from prison, compared to the general population. Image source: (NHS England, 2016b)
- Post-release mental health treatment and support is often poor (Criminal Justice Joint Inspectorate, 2021a):
- Nationally people leaving prison frequently face inappropriate delays when waiting to be contacted by community mental health services, and those who lack a fixed address before release often find it difficult to identify which services will provide their mental healthcare (Justice Committee, 2021).
- A 2006 study found the risk of dying by suicide for people recently released from prison is similar to that of people discharged from inpatient mental health wards (Richards, 2020).
- National data shows that more than 97% of the days offenders wore tags as part of Alcohol Abstinence and Monitoring Requirements (AAMRs) were alcohol free in 2021/22 (Hodges, 2022).
Additional resources
- The local data pack gives an overview of key data and trends
- A follow up of the 2009 Bradley Report reviewing the experience of people with mental health needs in the criminal justice system
- The Centre for Mental Health report on The future of prison mental health care in England
- Bromley Briefings Prison Factfile: Winter 2021
- The most recent needs assessment on this topic: Victims, Suspects and Offenders 2019/20
- Revolving Door’s report What next for Probation? Findings and recommendations from our Lived Experience Inquiry into Probation
- National Institute of Health Research’s summary of the importance of the criminal justice system within public mental health
- Cambridgeshire Insight data on Crime and Community safety
References
Full list of references is included at the end of this chapter.
