Local picture
Previous local strategies and reports have highlighted young adults’ access to mental healthcare as a priority. In particular, the Cambridgeshire and Peterborough’s Children and Young People’s Mental Health Strategy set ‘learning about the feasibility of services for 14-25- year olds’ and increasing mental health system capacity for 16- to 25- year olds as key priorities (Cambridgeshire and Peterborough Integrated Care System, 2022f). As part of this strategy:
- It was suggested that difficulties accessing mental health care may contribute to crisis support making up a high proportion of service contacts of young adults; and stated that more needs to be done to understand the capacity for treatment for mental health conditions in young adults
- Stakeholders highlighted concerns about transitions across age ranges and between systems, with young adults being reported to have the greatest difficulties accessing healthcare (which was perceived to be complicated and bureaucratic)
Similar concerns have been raised in other reports:
- The East of England Children and Young Person Mental Health Needs Assessment (2021) included ‘proactive transitions’ from children and young people’s mental health services to adult mental health services as a key priority (Pari, 2022).
- After the death of a young person by suicide in 2020, the local coroner raised concerns about the ‘gap between urgent and non-urgent services’ for vulnerable young adults and the barriers this age group faces to accessing support. This was highlighted as a key ongoing concern whilst the system plans to extend services to age 25 (Barlow, 2022).
- The Suicide Prevention Strategy highlights the importance of smooth transitions when entering adult mental health services, stating that: ‘considerable effort should be made when a young person enters adult services to ensure that the quality of care that they receive is consistent and suited to their needs’ (Cambridgeshire County Council, 2022).
Current picture of mental health services for young adults
Currently (in Summer 2023), the YOUnited referral hub is the single point of referral for mental health and emotional wellbeing support in Cambridgeshire and Peterborough. Children and young people are directed through support based on the i-THRIVE model. YOUnited accepts professional referrals for:
- Mental health and emotional wellbeing, up to age 17
- Suspected eating disorders, up to age 18
- Neurodevelopmental diagnoses, up to age 18
- Centre 33 (which provides one-to-one counselling and support), up to age 25
17- to 25-year-olds with suspected severe mental illnesses may fall through gaps in services and face a complicated route to accessing secondary mental health care. If they are not in contact with adult mental health services, including young adults who have not been through service transition from children and young people’s mental health services, they may feel they are being asked to repeat their stories multiple times. This cohort can only support by:
- Explaining their need for support to their GP
- Going through a consultation with another healthcare professional
- If accepted for treatment in adult services, waiting for an assessment with another mental health service
What does the data tell us?
Young people have multiple needs
Almost all young people seeking support from Centre 33, a local organisation that provides holistic support for young people up to the age of 25, have multiple needs. Out of the young people seeking support through the ‘Someone to Talk to’ service in 2021/22 (Centre 33, 2022):
- 93% have more than one need, with the most common need (92%) being around mental health
- 54% sought help with up to 8 different needs
- 40% sought help with issues around employment, housing and finances
- Almost 1 in 3 seeking mental health support were experiencing severe psychological distress
High levels of young adults present to services in mental health crisis
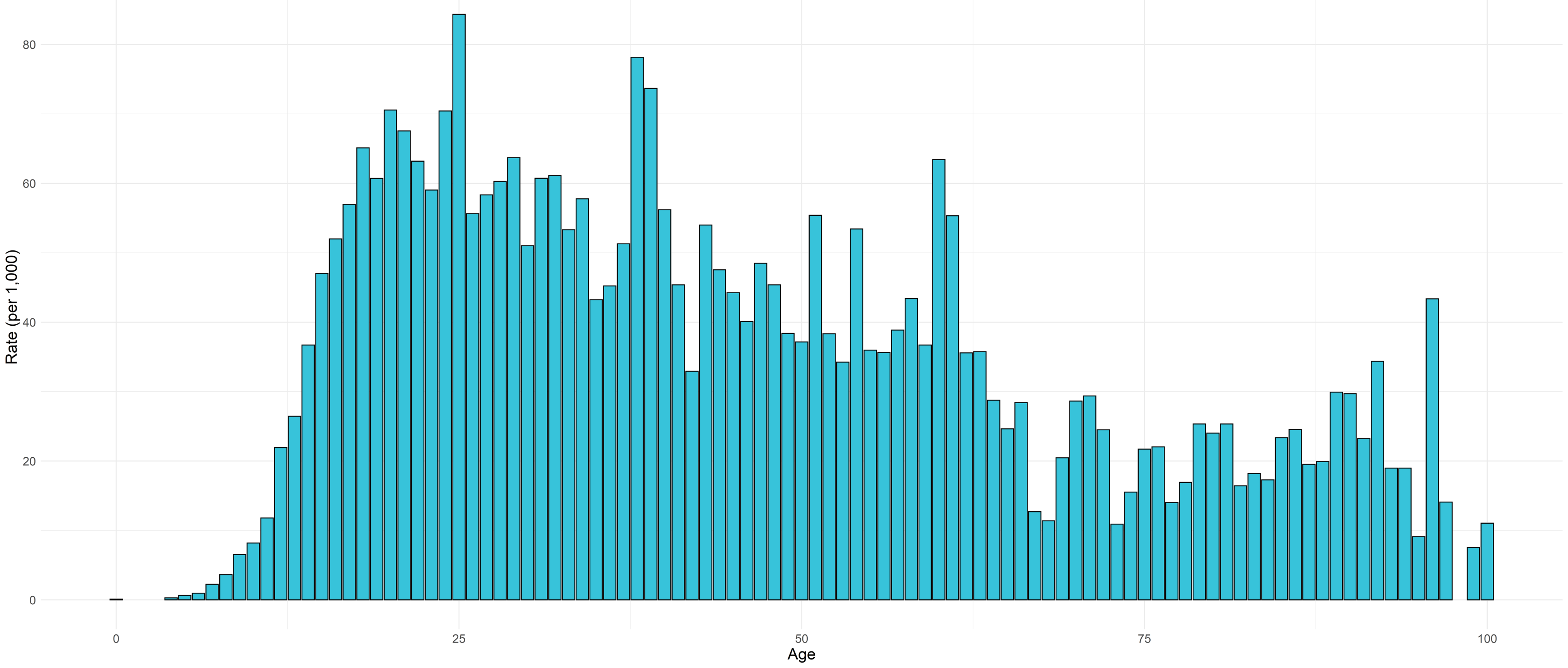
The First Response Service (FRS) provides support for people experiencing a mental health crisis and is available 24/7. Support offered can include telephone support, a face-to-face assessment and referral to other CPFT services. A detailed analysis of service use in FRS between August 2021 and March 2023 was carried out, which showed that there is an increasing rate of referrals from ages 15 to 18, with a sharp peak at age 25.
Figure 56: Age distribution of unique accepted referrals rate (per 1,000) to FRS, August 2021 – March 2023. Data source: FRS analysis
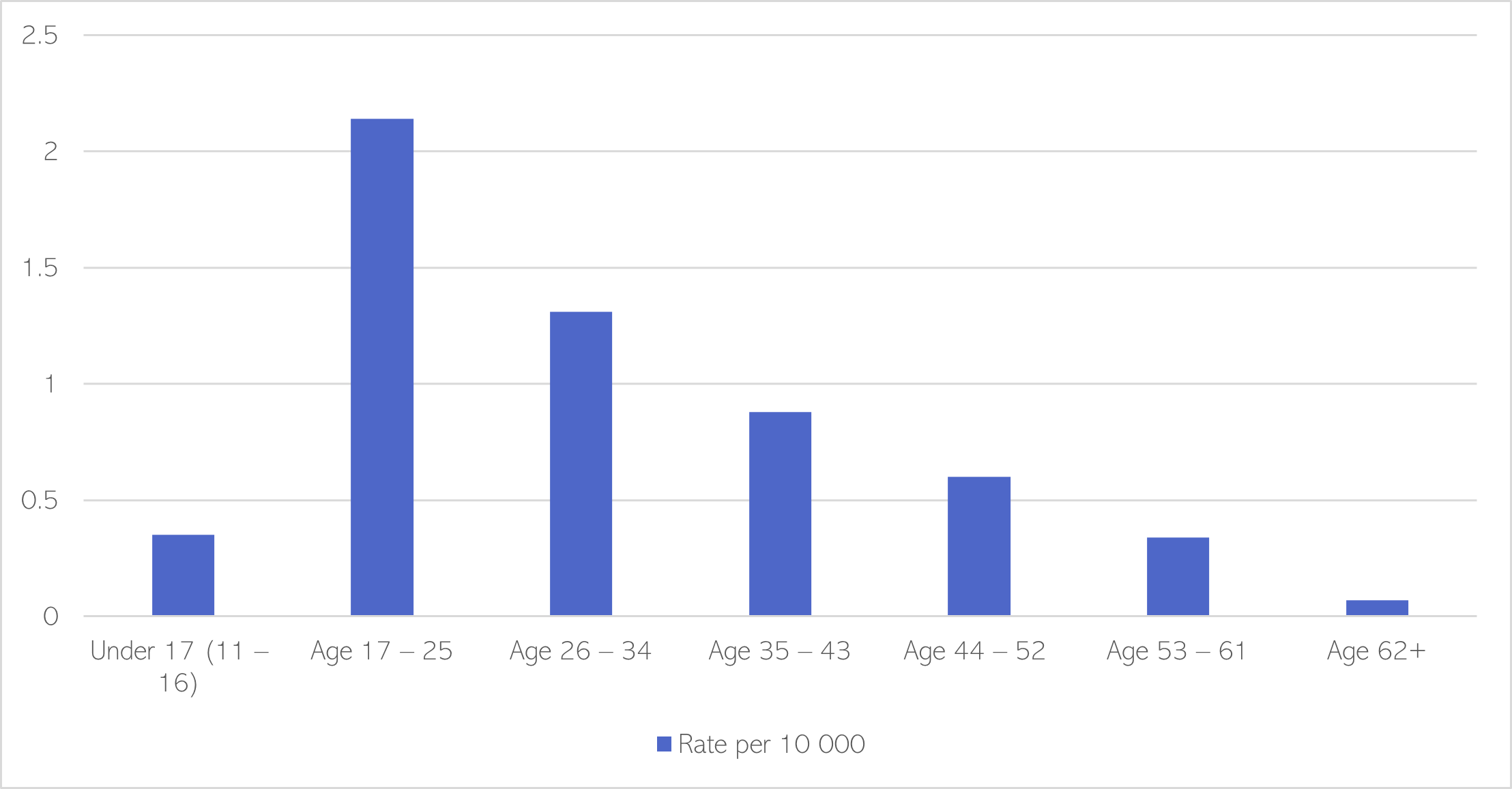
Similarly, young adults have the highest rate of detainment under Section 136 of the Mental Health Act. Section 136 is when police take or keep individuals at a ‘place of safety’.
Figure 58: Rate of Section 136 detainments in Cambridgeshire and Peterborough by age group, 2022/23
Patients attending Accident and Emergency services five or more times in the past year (May 2022 to April 2023) represent 0.45% of the population in Cambridgeshire and Peterborough but accounted for more than 1 in 10 (11.4%) of A&E attendances.
The most common chief complaint of young adults (aged 16 to 19) presenting at Accident and Emergency 5+ times in the past year is ‘psychosocial/behaviour’, which was the chief complaint in 20% of attendances. Repeat attendances may be a sign that people are not receiving appropriate care from services once they leave hospital.
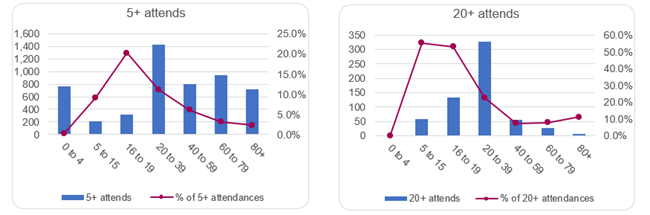
‘Psychosocial/behavioural’ factors were also the chief complaint for those attending Accident and Emergency 20+ times during the past year, across 5 to 15 year olds, 16 to 19 year olds, and 20 to 39 year olds. As shown below, this was particularly stark for young adults (aged 16 to 19) who attended Accident and Emergency 20+ times in the past year, for whom mental health attendances made up half of the reasons why people attended Accident and Emergency.
Figure 59: Mental health related attendances involving frequent A&E visitors. Data source: High Intensity Use Tool ICB (NHSE East of England)
What are young people’s experiences?
A report by Healthwatch Cambridgeshire and Healthwatch Peterborough, published in 2021, spoke to a very small sample of 8 young people and 5 parent carers about their experiences of transitions from children and adolescent’s mental health services to adult’s mental health services. This report found that:
- All of the people surveyed reported having been negatively impacted after facing difficult journey trying to access mental health support.
- Everyone surveyed reported having limited or no help navigating mental health service, with most families saying that they found it hard to understand the healthcare system. One parent stated: ‘we didn’t feel there was anybody on our side. We don’t know anything about the funding. There is a lot of hope at every step of this journey…but it just hasn’t worked out’.
- The majority of young people reported having little awareness of which mental health services were available to them, including little awareness of the Keep Your Head website.
- Everyone surveyed felt there was a lack of holistic care, with one parent stating ‘Nobody seems to stand back and think “what are this young person’s needs?’
- Many of the young people had experienced long waits to access child and adolescent mental health services. Some young people raised particular concerns around autistic people seeking mental health support for many years.
- Half the young people spoken to reported that not meeting the criteria for mental health services had been a difficulty for them. In some cases, young people reported becoming very unwell and in crisis and attending Accident and Emergency. Then they might meet the criteria to enter CAMHs or AMHs because they have deteriorated to such an extent.
References
Full list of references is included at the end of this chapter.