Migrants, asylum seekers and refugees
A large scale study found that migrants are 1.2 times more likely to report high levels of psychological distress in the postnatal period than non-migrants (44). A systematic review of systematic reviews about perinatal health among asylum seekers and refugees found that, compared to the general population, these groups are (71):
- Between 1.8 to 2.5 times more likely to experience postnatal depression.
- More likely to experience anxiety and PTSD during the perinatal period.
Local population
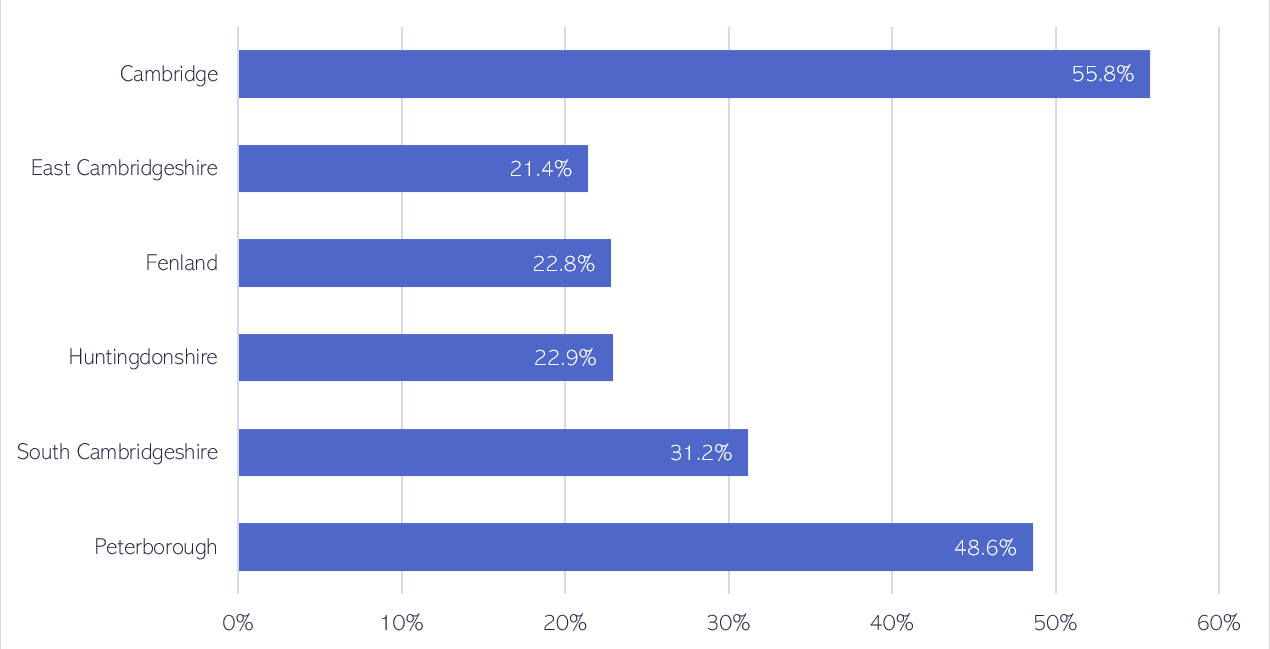
There is significant variation in the proportion of live births to non-UK-born women and birthing people across Cambridgeshire and Peterborough. The highest proportions are in Cambridge (55.8%) and Peterborough (48.6%). The national average is 29.6%.
Figure 11: Percentage of live births born to non-UK-born women by local authority district, in 2021. Data source: (70)
Risk factors for poor mental health
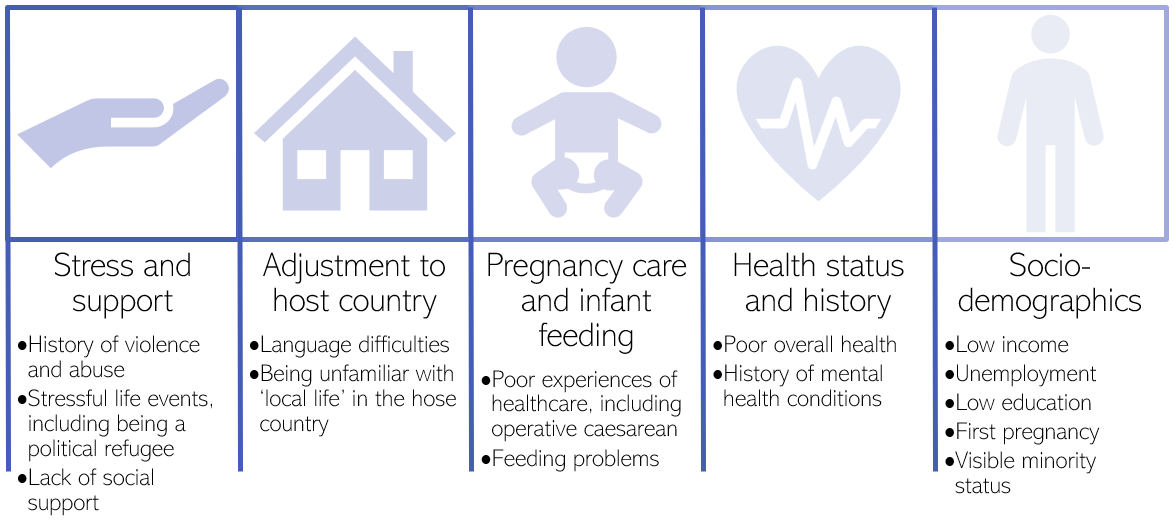
Risk factors for perinatal mental health conditions amongst people seeking asylum and refugees include:
Figure 12: Factors associated with an increased risk of perinatal mental health conditions in people seeking asylum and refugees. Adapted from: (71)
Refugees and people seeking asylum are also at higher risk of preterm births, having infants with congenital abnormalities and maternal mortality (71).
Access
Compared to non-migrants, migrants are less likely to access perinatal mental health support (71), and are half as likely to receive treatment for postnatal anxiety or depression (44). Specific barriers to accessing care faced by migrants in the perinatal period are similar to those included in chapter 2 (71). Asylum seekers and refugees face many similar barriers to migrants, as well as:
- Mistrust of healthcare professionals, who can be perceived as a threat to the safety of asylum seekers who do not engage with care (71).
- Dispersal (movement to asylum accommodation in a different part of the UK), which can disrupt continuity of care and is associated with late booking for antenatal care (72).
- The policy of charging undocumented migrants for maternity care (60,71).
Impact of charges for NHS care (73)
- People who have been refused asylum, have No Resource to Public funds (NRPF) or are living in the UK without official immigration status may be charged for hospital-based care.
- Evidence suggests that this deters people from accessing maternity care. Some women also report high levels of stress and anxiety around these charges.
- Bills following birth generally start at around £7,000; but can rise to tens of thousands for complex births. The NHS has an obligation to report unpaid debts of £500 or more to the Home Office, which can threaten future immigration applications.
- Charging may increase women’s vulnerability to domestic violence, and places them at increased risk of exploitation and abuse.
Experience
An umbrella review of studies found that migrants are less positive about their perinatal care than non-migrants, particularly in relation to mental health (71). Common themes included:
Figure 13: Common themes in migrants, asylum seekers and refugees’ experiences of perinatal care. Data source: (71).
A systematic review of systematic reviews found that people seeking asylum and refugees report similar experiences to migrants, with the most vulnerable women in these groups having the most negative interactions with healthcare professionals, including discriminatory care, cultural stigma and stereotyping (71).
Additional resources
- Review of the evidence on the effects of the social determinants of mental health on migrants is in the paper: The social determinants of mental health and disorder: evidence, prevention and recommendations.
- Starting Well – Perinatal Mental Health Support for Muslim Communities captures the experiences of Muslim mums in Peterborough
- Embedding cultural awareness in maternity services
- Royal College of Midwives pocket guide on Caring for vulnerable migrant women
- British Medical Association Refugee and asylum seeker patient health toolkit
- Maternity Action’s guidance on Improving access to maternity care for women affected by charging
References
70. Office for National Statistics. Births by parents’ country of birth, England and Wales: 2021 [Internet]. 2022 [cited 2023 Mar 30]. Available from: https://www.ons.gov.uk/peoplepopulationandcommunity/birthsdeathsandmarriages/livebirths/bulletins/parentscountryofbirthenglandandwales/2021#:~:text=There%20were%20445%2C055%20live%20births,UK%2Dborn%20women%20in%202021.
71. Heslehurst N, Brown H, Pemu A, Coleman H, Rankin J. Perinatal health outcomes and care among asylum seekers and refugees: A systematic review of systematic reviews. BMC Med. 2018;16(1).
72. Gibbons-Arif H. Equality and the asylum system: the case of pregnant women [Internet]. Maternity Action. 2021 [cited 2023 Feb 17]. Available from: https://maternityaction.org.uk/2021/11/equality-and-the-asylum-system-the-case-of-pregnant-women/
73. Breach of Trust: a review of the implementation of the NHS charging programme in maternity services in England [Internet]. 2021 [cited 2023 Feb 17]. Available from: https://maternityaction.org.uk/breach-of-trust-report-2021/